<30312E20C6AFC1FD303220B1E8C8A3B0A22E687770>
|
|
|
- 기영 이
- 7 years ago
- Views:
Transcription
1 대한내과학회지 : 제 78 권제 3 호 2010 특집 (Special Review) - 췌장의낭종성질환 췌장의낭종성질환의감별진단 대구가톨릭대학교의과대학내과학교실 김호각 Differential diagnosis of cystic diseases of pancreas Ho Gak Kim, M.D., Ph.D. Department of Internal Medicine, Catholic University of Daegu School of Medicine, Daegu, Korea Cystic diseases of pancreas are increasingly detected because of high quality of imaging modality. Most of pancreatic cysts are discovered incidentally. Differential diagnosis of pancreatic cysts is very important because they include wide range of pathologic disease such as inflammation, benign neoplasm, borderline and malignant neoplasm. The most common cystic disease of pancreas is post-inflammatory pseudocyst, but in recent decades the incidence of neoplastic cysts, such as serous cyst neoplasm, mucinous cyst neoplasm, intraductal papillary mucinous neoplasm has increased. Among the cystic neoplasms, mucinous cystic neoplasm, intraductal papillary mucinous neoplasm are premalignant, and serous cystadenoma has no malignant potential. Patient s age, symptoms and a possible history of acute or chronic pancreatitis together with cross-sectional imaging modalities are mainstay for differential diagnosis of cystic diseases of pancreas. Cystic fluid cytology and analysis for CEA, mucin stain, and viscosity are providing additional information for differentiation. But cross-sectional images have overlapping findings in various cystic diseases and cystic fluid aspiration has still lack of sensitivity. The purpose of this review article is to provide the overview of the differentiation of pancreatic cystic lesions. (Korean J Med 78: , 2010) Key Words: Cystic disease; Pancreas; Diagnosis, differential 서론췌장의낭종성질환 (cystic disease) 은낮게는초음파선별검사에서 0.2% 로보고되며, 높게는부검에서 24.3% 까지보고되고있다 1). 영상진단에서췌장낭종의발견은그진단방법에따라그차이가크며최근영상진단기기나기술의발전으로그보고빈도가점차높아지고있다 2,3). 대부분의췌장낭종성질환은증상이없이우연히발견되며 2~3년이지나도변화가없이지속된다 4). 다른한편으로는췌장낭성질환중일부는악성변화를할수있으며, 발전된영상진단에의해발견당시에악성이의심되어서수술치료를받는경우가증가하고있다. 그러나수술전낭성질 환의정확한진단이어려운경우가있으며수술전과수술후의진단이불일치하는경우도많다. 이논평에서는췌장낭종성질환중에서비교적흔한종류인가성낭 (pseudocyst), 점액성낭종 (mucinous cyst neoplasm), 장액성낭종 (serous cyst neoplasm), 관내유두상점액성종양 (intraductal papillary mucinous neoplasm, IPMN) 그리고고형가성유두상종양 (solid pseudopapillary tumor) 을중심으로췌장낭종성질환의감별을알아보고자한다. 췌장낭종성질환의분류췌장의낭종성질환의분류는여러방법이있으나임상적
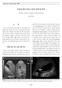
2 - The Korean Journal of Medicine: Vol. 78, No. 3, Table 1. WHO classification of cystic neoplasms of the pancreas Serous microcystic adenoma Serous oligocystic adenoma Serous cystadenocarcinoma Mucinous cystadenoma Mucinous cystic tumor-borderline Mucinous cystadenocarcinoma Non-invasive Invasive Intraductal papillary mucinous adenoma Intraductal papillary mucinous neoplasm- borderline Intraductal papillary mucinous carcinoma Non-invasive Invasive 으로흔히쓰이는유용한분류로는낭종의병리학적구분에따라잔류낭종 (retension cyst), 가성낭 ( 거짓낭 ) 그리고낭종성종양으로나누며, 낭종성종양은구체적으로 WHO 분류가있다 ( 표 1) 5,6). 잔류낭종혹은진성낭종 (true cyst) 은정상췌관세포나췌장선방세포 (centroacinar cell) 로구성되고췌액이고인적은크기의낭을말하며임상적으로문제가없다 ( 그림 1). Von Hippel-Lindau 병도일종의선천성의진성낭종으로다발성으로췌장에여러크기의낭종이동반된다 ( 그림 2). 가성낭은췌장의염증이나괴사의결과로췌장실질안이나밖으로염증성삼출액이나췌액이고이는것으로췌장효 소를많이함유하고있으며낭벽은점막세포가없이섬유조직, 육아조직으로되어있다. 낭종성종양은 WHO 분류을중심으로일반적으로단순히점액성낭선종 (mucinous cystadenoma) 혹은점액성낭선암 (mucinous cystadenocarcinoma), 췌장의관내유두상점액성종양, 장액성낭종, 고형가성유두상종양으로나눈다 ( 표 2) 6). 이중장액성낭종은췌장의선방세포에서발생하는양성종양으로낭종의내면이얇은점막으로구성되며낭내에맑은장액이고이게되며 ( 그림 3), 점액성낭종은점액을분비하는원주상피세포 (mucin-producing columnar epithelium) 로구성되며난소형기질 (ovarian type stroma) 을가지는경우가있으며낭종의내층세포가점액을분비하여낭내에점액이고이게되며 ( 그림 4), 관내유두상점액성종양은췌관에서발생한유두상종양에서점액이분비되어역시췌관에점액이고여서낭모양으로확장되는것이며 ( 그림 5), 고형가성유두상종양은고형의종양이낭성병성 (cystic degeneration) 혹은괴사에의해낭종으로변하면서내면이유두양을보이는것으로낭종의내면은유두양세포와점액양기질 (myxoid stroma) 을가진다 ( 그림 6). 이중서양에서는점액성낭종이가장흔하며 7), 일본이나우리나라에서는 IPMN 이흔하며국내의다기관조사에서도 IPMN 이가장흔하고이어서가성낭, 점액성낭종, 장액성낭종순의빈도였다 8). 여기서는췌장의낭종성질환중흔한형태인가성낭, 점액성낭종, 장액성낭종, IPMN 그리고고형가성유두상종양의감별해보고자한다. Figure 1. Retension cyst of pancreas body. Figure 2. Pancreas cysts in the patient with von Hippel-Lindau disease. There are multiple cysts in body of pancreas
3 - Ho Gak Kim. Differential diagnosis of cystic diseases of pancreas - Table 2. Cystic lesions of pancreas classified according to lining of cyst No lining Pseudocyst Mucinous epithelium Mucinous cyst neoplasm Intreductal papillary mucinous neoplasm Serous (clear cell) epithelium Serous cystadenoma Von Hippel-Lindau syndrome Acinar cell Acinar cell carcinoma (cystic endocrine tumor) Degenerative changes of solid tumor Solid pseudopapillary tumor Cystic ductal adenocarcinoma 췌장낭종성질환의감별진단 1. 임상특성과증상에의한감별 1) 성별과연령에의한감별가성낭은지역과연령에따라차이가있지만췌장의낭종성질환중가장흔한것으로대부분알코올성췌장염에서생기므로음주력이있는남자에서흔하며담석증등다른원인의췌장염이나췌장손상의병력이있는사람에서도의심할수있다. 장액성낭종은양성종양으로악성변화를거의하지않는것으로남성에서도생길수있으나주로고령층의여성에흔하다. 점액성낭종은대부분중년여성에서생기며크기가커지면서악성화의가능성이매우크다. IPMN 은남녀의발생이비슷하며증상이없이서서히커지므로고령에서발견이많이되고서양의보고보다우리나라 Figure 3. Cartoon of serous cyst neoplasm of pancreas. Cystic mass are composed of clusters of multiple small cysts with stellate scar in septa (quoted from The Pancreas, Berger HG, eds, Blackwell Science, London 1998). Figure 4. Cartoon of mucinous cyst neoplasm of pancreas. Cystic mass are surrounded by thick irregular wall and divided with thick septa (quoted from The Pancreas, Berger HG, eds, Blackwell Science, London 1998). Figure 5. Cartoon of intraductal papillary mucinous neoplasm of pancreas. Mucing producing papillary mass are arising along epithelium of pancreatic duct with cystic dilatation (quoted from The Pancreas, Berger HG, eds, Blackwell Science, London 1998). Figure 6. Cartoon of solid pseudopapillary tumor in pancreas. The mass has solid and cystic portions concomitantly (quoted from The Pancreas, Berger HG, eds, Blackwell Science, London 1998)
4 - 대한내과학회지 : 제 78 권제 3 호통권제 595 호 Table 3. Differential diagnosis of pancreatic cystic diseases Type Age Gender Cyst fluid Serous cystadenoma Older F>M Tin, serous, often bloody Mucinous cystic neoplasm Intraductal papillary mucinous neoplasm Solid pseudopapillary tumor Pseudocyst Middle age F>>M Mucoid, often viscus Older M=F Mucoid, often viscus Amylase activity Cystic fluid analysis CEA Viscosity Mucin stain Cytology Negative Glycogen-rich cell Positive Mucinous cell Positive Mucinous cell Young F>M Bloody Negative Epithelial cell, necrotic cell Variable range M>F Prune color, often bloody Negative, decrease mildly;, increased markedly;, increased moderately;, increased mildly;, normal range. Inflammatory cell Table 4. Clinical features of cystic lesions of pancreas Etiology Type Malignant potential Communication with duct Congenital Retention cyst None Seldom Post-inflammatory Pseudocyst None Frequent Neoplastic Serous cysadenoma Very low Rarely Mucinous cystadenoma High Occasionally IPMN High Yes Solid pseudopapillary neoplasm Moderate Occasionally IPMN, intraductal papillary mucinous neoplasm. 에서더흔하다 8). 고형가성유두상종양은비교적드문종양으로고형유두상상피종양 (solid papillary epithelial neoplasm) 으로도불리며젊은여성에서상당히큰종괴로발견되는경우가많다 ( 표 3). 2) 증상에의한감별대부분의췌장낭종성질환은증상이없이우연히발견된다. 낭종성병변자체가복통, 췌장염, 염증에의한고열, 담관폐쇄에의한황달을일으킬수있으나대부분증상이없다. 가성낭은최근의췌장염의병력이있는경우나혈청아밀라제나리파제가증가한경우에의심하여야하며, 이미만성췌장염으로진단된환자이거나영상진단에서췌장에서만성췌장염에합당한소견인췌장의석회화, 췌관의협착과확장및췌관결석이있는경우도가성낭을의심할수있다. 관내유두상점액성종양도때로는점액에의한췌관폐쇄로췌장염이생길수있다. 점액성낭종과장액성낭종도크기가매우커서췌관이나담관을막을경우에는췌장염이나 폐쇄성황달이생길수있다. 점액성낭종과관내유두상점액성종양이악성변화를하여췌장에악성종괴를형성하거나주변조직으로의침윤이나전이가있으면복통, 식욕부진, 체중감소등증상이있을수있다 ( 표 4). 2. 영상학진단에의한감별췌장의낭성병변을진단하기위한여러가지영상진단법으로는비침습적으로단면상 (cross-sectional image) 을얻는것으로복부초음파, 전산화단층촬영 (computed tomogram, CT), 자기공명영상 (magnetic resonance imaging, MRI) 이있으며침습적인방법으로내시경역행담췌관조영술 (endoscopic retrograde cholangiopancreatography, ERCP) 및내시경초음파 (endoscopic ultrasonography, EUS) 가있다여기에서는복부초음파, CT, MRI 및 ERCP 소견으로췌장의낭종성질환을감별하는것을알아보겠다 ( 표 4, 5)
5 - 김호각. 췌장의낭종성질환의감별진단 - Table 5. Differentiation of cystic lesion of pancreas according to cyst morphology Cyst morphology Diagram of cyst Included cystic diseases Unilocular Pseudocyst Cystic degeneration of ductal adenocarcinoma Cystic endocrine tumor Retention cyst, von Hippel-Lindau syndrome Microcystic Serous cystadenoma Cystic endocrine tumor von Hippel-Lindau syndrome Macrocystic Mucinous cystadenoma Intraductal papillary mucinous neoplasm Serous macrocystic adenoma Solid component in cyst Solid pseudopapillary tumor Cystic degeneration of malignant neoplasm Figure 7. CT scan of pancreatic pseudocyst. There is large exophytic cystic lesion at body of pancreas with severe inflammation at tail of pancreas. Figure 8. CT scan of serous cystadenoma. There is microcystic cystic mass with central stellate septa at body of pancreas. 1) 가성낭가성낭은췌장내에생기는모든낭종성병변의 70% 를차지한다 9). 초음파나 CT에서췌장에급성췌장염혹은만성췌장염의소견이있으면서주로단방성 (unilocular) 의낭성종괴가췌장밖으로돌출해있는형태이며, 낭벽은보통 4 mm 미만으로얇게 CT에서조영되며주변에염증소견이같이있다 ( 그림 7). 종괴에고형부분이없으며낭액은내용물 이없는췌액이거나찌꺼기가아래쪽에침전되어있거나출혈이동반되어있기도한다. ERCP나 MRI에서주췌관과교통이있는경우가 65~70% 이다 9). 2) 장액성낭종장액성낭종은췌장머리에서많이생기지만췌장몸체, 꼬리에서도관찰된다. 가장흔한형태로는 70% 에서 2 cm 미
6 - The Korean Journal of Medicine: Vol. 78, No. 3, Figure 9. Endoscopic retrograde pancreatography of serous cystadenoma. Main pancreatic duct was displaced by large cystic mass at head of pancreas. Figure 10. CT scan of mucinous cystic neoplasm. There is medium-sized cystic mass with thick wall and eccentric septum at tail of pancreas. Figure 11. CT scan of intraductal papillary mucinous neoplasm. Main pancreatic duct was dilated with enhancing mural mural at head of pancreas. 만의작은낭들이 6~7개이상여러개가뭉쳐서 5 cm 미만의하나의다방성 (multilocular) 낭을만들어 (microcystic serous cystadenoma) 스폰지모양을하고있으며특징적으로가운데에별모양의석회화가동반된반흔을가지고있다 ( 그림 8) 10). 태양불꽃 (sunburst) 모양의가운데의석회화가장액성낭종의 30% 에서볼수있으며이는장액성낭종의진단적특징이다 11). 장액성낭종의장벽은얇고낭액은내용물이없는장액으로되어있다. 장액성낭종의 20% 에서는 1 mm 이하의낭들이뭉쳐서영상진단에서하나하나의낭을구별하기가어려워서벌집모양혹은고형종양처럼보이지만초음파및 CT에서는저에코및저음영으로보이며 MRI에서 T2- 조영증강에서높은신호강도를보인다. 각각낭의크기가 0.5~1.0 cm 이상인여러낭이모여서된장액성낭종 (macrocystic 혹은 oligicystic serous cystadenoma) 는 10% 미만으로형태적로는점액성낭종이나중격이있는가성낭과구별이어렵다. 장액성낭종은췌장내에있으며주변췌장조직과경계가명확하고췌관과교통이없으며크기가크면췌관이나담관을외부에서압박할수있다 ( 그림 9). 3) 점액성낭종점액성낭종은췌장의몸체나꼬리에주로있으며 4~5 cm 이상의비교적큰크기이며때로는 25 cm까지되기도한
7 - Ho Gak Kim. Differential diagnosis of cystic diseases of pancreas - A B Figure 12. CT scan and magnetic resonance cholangiopancreatography of branch-type intraductal papillary mucinous neoplasm. There is cystic dilatation of branch ducts at uncinate process of pancreas on CT scan (A). On magnetic resonance cholangiopancreatography, dilated ducts look like bunch of grape having communication with main pancreatic duct (B). 다 11). 낭은두껍고불규칙한섬유성벽으로둘러싸여있으며중격에의해여러개의방으로나누어져있으나일반적으로 6개미만이며주변에작은크기의인접한낭들이있기도하다 ( 그림 10) 12,13). 점액성낭종은보통췌관과교통이없으며크기가커서췌관을막을수있다. 장액성낭종과크기로감별은어려우나불규칙하고두꺼운낭벽에유두양돌기가있고낭내로뻗어있는중격과같은내부구조로점액성낭종을진단할수있다. 가성낭과의감별은낭종주변에염증소견이없으며췌실질에도급성췌장염이나만성췌장염의소견이없고대신에중격이흔히보이고낭액이점액이어서내용물의에코나밀도가높다. 점액성낭종에서낭내에조영이되는종괴가있거나낭벽에서계란모양의석회화가있으면점액성낭선암을의심할수있다 14,15). 4) 췌장의관내유두상점액성종양 IPMN 은췌관내의점액분비성종양세포에서분비되는점액의높은점성때문에췌관이미만성혹은국소적으로확장되며때로는췌관이낭종의형태로확장되는특징이있다. IPMN 은주췌관형 IPMN 과분지관형 IPMN 으로분류되며 16,17) 주췌관형은주췌관을미만성으로혹은국소적으로침범하며주로췌장의머리쪽에서시작하며몸체와꼬리방향으로진행한다. 분지관형은더젊은나이에발생하고췌장머리의갈고리돌기 (uncinate process) 에서잘생기며꼬리에 Figure 13. Fish-eye appearance of major papilla in intraductal papillary mucinous neoplasm. Clear mucin is dropping from patulous major papilla. 서발생하기도한다. 주췌관형과분지관형이합쳐진경우도있다. 췌장조영 CT는췌관의확장이나낭성종양을확인할수있어서 IPMN 의선별에가장좋은진단방법이며종양세포들이종괴를형성하고있어서조영이되는벽성결절 (mural nodule) 을볼수도있다 ( 그림 11). 분지형 IPMN 에서는주췌관의확장이없이도분지관의확장을볼수있다 ( 그림 12A)
8 - 대한내과학회지 : 제 78 권제 3 호통권제 595 호 A B Figure 14. CT scan and endoscopic retrograde pancreatography of malignant intraductal papillary mucinous neoplasm. There is enhancing mass in the dilated main pancreatic duct on CT (A) and filling defect at endoscopic retrograde pancreatography (B) at body and tail of pancreas. 자기공명담췌관조영술 (magnetic resonance cholangiopancreatography, MRCP) 은점액이고여있어서확장되어있는췌관의범위를 ERCP보다는더민감하게보여주며분지관형의경우도쉽게주췌관과교통하는지알수있다. 분지형의경우는 MRCP에서낭성종양이포도송이모양으로보인다 ( 그림 12B). IPMN 의진단에서 MRCP 는 CT와같거나더우월하며 18), IPMN 의상태의판단에서도 ERCP에서는점액마개 (mucus plug) 에의해췌관이막히므로 MRCP가더민감하다 19). IPMN 의특징적인 ERCP 소견은주로 IPMN 병소가있는부분의하류쪽, 즉유두방향의췌관이특별한협착이없이점액의저류로인한미만성혹은국소적으로확장되어있으며심해지면근처의분지까지확장된다. 점액이나벽성결절로인해충만결손이보이기도한다. 내시경소견에서유두가확장되어물고기눈모양 (fish-eye) 모양을하며때로점액이흘러나오기도한다 ( 그림 13). 분지관형의경우는조영제가채워지면서낭성확장을볼수있다. IPMN 에서악성변화를시사하는소견으로는 (1) 주췌관형에서 10 mm 이상의췌관확장이있거나 (2) 분지관형에서전체낭종의크기가 30 mm 이상이거나중격이불규칙하거나두꺼워져있거나 (3) 벽성결절이 3 mm 이상으로보이는경우다 ( 그림 14) 20,21). IPMN 을점액성낭종과감별하는방법으로는주췌관이나분지관이확장되어있으며확장된췌관에점액마개나벽성결절이보이며분지형에서도 MRCP나 ERCP에서낭성으로확장된분지관이주췌관과교통이있는것으로진단할수 Figure 15. CT scan of large solid pseudopapillary tumor at tail of pancreas. The mass has large degenerative cyst and solid component with calcification. 있다. 5) 고형가성유두상종양고형가성유두상종양은고형종양으로시작하여낭성변성을초래하는것으로낭내에는출혈, 괴사조직, 탐식세포등이있으며, 영상조영에서 10 cm 이상의비교적큰크기의경계가명확한종괴가췌장의어느부위에서나발견될수있다 ( 그림 15) 15). 종괴내에는고형과낭성부분이같이있는경우가많으며석회화가흔히동반된다. 혈류가풍부하여출혈이동반되기도한다. 고형부분과낭성부분이교차로존재
9 - 김호각. 췌장의낭종성질환의감별진단 - 하는것이진단에특징적이다. 3. 낭액의천자에의한감별췌장의낭종성질환은낭액을천자하여낭액의육안적소견, 생화학적분석, 점도검사, 종양표지자검사, 세포검사등으로감별을시도할수있다. 췌장낭종의천자는복부초음파나 CT를이용한경피적천자로할수도있으며최근에는 EUS를이용한세침흡입술 (fine needle aspiration, FNA) 로낭액의분석이나세포검사를많이하고있다 ( 표 3). 1) 세침흡인액의세포검사췌장낭종의천자액세포검사의가장큰단점으로는췌장낭종액에는세포수가적어서진단이어렵고민감도가낮다 14). 악성변화가있을때에민감도가올라가지만악성점액성낭종에서도 29% 정도이다 23). 그러나악성낭종에서특이도는매우높다. 낭액의천자액에서가성낭과점액성낭종의감별은점액소염색 (mucin stain) 이나점도 (viscosity) 의측정에서양성이나오면점액성낭종으로진단할수있다. 가성낭에서는염증세포가있으나상피세포는보이지않고점액과점도도없다. 낭종의감별을위한천자액의세포검사에서점액세포가보이지않고일정한모양의췌관의선방근처의세관세포 (ductule cell) 에해당하는상피세포가끊어져보이면장액성낭종으로진단할수있으며점액세포가보이면점액성낭종이나 IPMN 으로진단할수있지만대부분감별이어렵다. 2) 세침흡인액의분석췌장낭성병변에서의낭액의분석은어느정도진단적가치가있다 ( 표 3). 가성낭의낭액은아밀라제치가매우높을수있으나점액소염색에서음성이며점도측정에서양성을보이지않는다. 장액성낭종은점액소가없으며글리코겐 (glycogen) 에대한 PAS 염색에서양성을보인다. 낭액은아밀라제나 CA19-9, CEA의증가가없다. 점액성낭종과 IPMN 에서는천자액에서점액소염색이양성이며 CEA가증가한다. 특히 CEA가 250 ng/ml 이상이면점액성낭종을진단할수있으며 5 ng/ml 미만이면제외할수있다 24,25). 차단 (cut-off) 수치를 400 ng/ml으로하면점액성낭종을가성낭과감별할때민감도가 57%, 특이도가 100% 였다 25). 다른종양표지자인 CA 19-9, CA 125, CA 72-4 등도점액상낭종에서증가되어있으나진단가치는낮다. 낭액의 CA19-9 나 CEA의증가는양성보다악성점액성낭종이나악성 IPMN 에서더흔히볼수있다 26). 천자액의아밀라제치는감별진단에서낭종의감별에큰감별은되지않으나아밀라제치가많이높은경우는가성낭을강하게의심할수있으나 IPMN 에서도역시많이증가되어있으며점액성낭종이췌관과교통하고있는경우도증가하며, IPMN 도췌관과교통이없이오래지속된경우는아밀라제치가증가하지않는다. 췌장낭의천자액에서점도의증가는점액소의존재를의미하며점액성낭종이나 IPMN 을의미한다. 맺음말췌장낭종성질환은염증성질환에의한낭종부터악성낭종까지그범위가다양하지만여러가지방사선및내시경진단방법이개선되고, 낭액의 FNA와같은새로운진단방법이소개되어도정확한진단과감별이어려운경우가있다. 췌장낭종성질환이증상의유무와관계없이영상진단에서발견되면다음과같은사항을염두에두어야하겠다. 첫째, 췌장의낭종은크기나증상의유무에관계없이진단을위한평가를시행하여야한다. 둘째, 췌장의낭종성질환중점액성낭종과 IPMN 은악성화의가능성이있으며드문질환인고형가성유두상종양도악성이될수있다. 셋째, 췌장낭종성질환의영상진단의첫째선택은조영증강 CT이며추가감별을위해서 EUS나 MRCP가가능한 MRI 를추천할수있다. 넷째, 낭액의세포검사는낭종의감별에도움이되지않으나, 점액성낭종이의심되면 EUS-FNA를이용한낭액의 CEA 검사, 점액소염색, 점도검사로감별에도움을준다. 다섯째, IPMN 이의심이되는경우는 MRCP, ERCP를통해췌관과의교통을확인할수있으며 ERCP에서유두에서점액분비를확인하는것이진단특이성이되며 MRCP에서는 IPMN 의범위를알수있다. 여섯째, 여러가지진단방법을동원하여도감별이불가능한경우가있으며장액성낭종이나잔류낭종이라고확신하지않는경우는정기적인추적이필요하다. 중심단어 : 췌장 ; 낭종성질환 ; 감별진단
10 - The Korean Journal of Medicine: Vol. 78, No. 3, REFERENCES 1) Ikeda M, Sato T, Morozumi A, Fujino MA, Yoda Y, Ochiai M, Kobayashi K. Morphologic changes in the pancreas detected by screening ultrasonography in a mass survey, with special reference to main duct dilatation, cyst formation, and calcification. Pancreas 9: , ) Kimura W, Nagai H, Kuroda A, Muto T, Esaki Y. Analysis of small cystic lesions of the pancreas. Int J Pancreatol 18: , ) Ferrone CR, Correa-Gallego C, Warshaw AL, Brugge WR, Forcione DG, Thayer SP, Fernandez-del Castillo C. Current trends in pancreatic cystic neoplasms. Arch Surg 144: , ) Das A, Wells CD, Nguyen CC. Incidental cystic neoplasms of pancreas: what is the optimal interval of imaging surveillance? Am J Gastroenterol 103: , ) Garcea G, Ong SL, Rajesh A, Neal CP, Pollard CA, Berry DP, Dennison AR. Cystic lesions of the pancreas. A diagnostic and management dilemma. Pancreatology 8: , ) Hamilton SR. Aaltonen LA (eds). Pathology and genetics of tumors of the digestive system. World Health Organization classification of tumors. Lyon, IARC Press, ) Grieshop NA, Wiebke EA, Kratzer SS, Madura JA. Cystic neoplasms of the pancreas. Am Surg 60: ; discussion , ) 윤원재, 윤용범, 이광혁, 이준규, 이우진, 류지곤, 이규택, 문영수, 이동기, 최호순, 김용태, 박찬국, 김호각, 김명환, 김진홍, 설상영, 유종선, 김창덕, 심찬섭, 정재복. 한국에서의췌장의낭성종양. 대한내과학회지 70: , ) Singhal D, Kakodkar R, Sud R, Chaudhary A. Issues in management of pancreatic pseudocysts. JOP 7: , ) Johnson CD, Stephens DH, Charboneau JW, Carpenter HA, Welch TJ. Cystic pancreatic tumors: CT and sonographic assessment. AJR Am J Roentgenol 151: , ) Sakorafas GH, Sarr MG. Cystic neoplasms of the pancreas; what a clinician should know. Cancer Treat Rev 31: , ) Sarr MG, Murr M, Smyrk TC, Yeo CJ, Fernandez-del-Castillo C, Hawes RH, Freeny PC. Primary cystic neoplasms of the pancreas. Neoplastic disorders of emerging importance-current state-ofthe-art and unanswered questions. J Gastrointest Surg 7: , ) Kimura W, Sasahira N, Yoshikawa T, Muto T, Makuuchi M. Duct-ectatic type of mucin producing tumor of the pancreas--new concept of pancreatic neoplasia. Hepatogastroenterology 43: , ) Lewandrowski KB, Southern JF, Pins MR, Compton CC, Warshaw AL. Cyst fluid analysis in the differential diagnosis of pancreatic cysts. A comparison of pseudocysts, serous cystadenomas, mucinous cystic neoplasms, and mucinous cystadenocarcinoma. Ann Surg 217:41-47, ) Campbell F, Azadeh B. Cystic neoplasms of the exocrine pancreas. Histopathology 52: , ) Kobari M, Egawa S, Shibuya K, Shimamura H, Sunamura M, Takeda K, Matsuno S, Furukawa T. Intraductal papillary mucinous tumors of the pancreas comprise 2 clinical subtypes: differences in clinical characteristics and surgical management. Arch Surg 134: , ) Terris B, Ponsot P, Paye F, Hammel P, Sauvanet A, Molas G, Bernades P, Belghiti J, Ruszniewski P, Flejou JF. Intraductal papillary mucinous tumors of the pancreas confined to secondary ducts show less aggressive pathologic features as compared with those involving the main pancreatic duct. Am J Surg Pathol 24: , ) Fukukura Y, Fujiyoshi F, Hamada H, Takao S, Aikou T, Hamada N, Yonezawa S, Nakajo M. Intraductal papillary mucinous tumors of the pancreas. Comparison of helical CT and MR imaging. Acta Radiol 44: , ) Sugiyama M, Abe N, Tokuhara M, Masaki T, Mori T, Takahara T, Hachiya J, Atomi Y. Magnetic resonance cholangiopancreatography for postoperative follow-up of intraductal papillary- mucinous tumors of the pancreas. Am J Surg 185: , ) Cellier C, Cuillerier E, Palazzo L, Rickaert F, Flejou JF, Napoleon B, Van Gansbeke D, Bely N, Ponsot P, Partensky C, Cugnenc PH, Barbier JP, Deviere J, Cremer M. Intraductal papillary and mucinous tumors of the pancreas: accuracy of preoperative computed tomography, endoscopic retrograde pancreatography and endoscopic ultrasonography, and long-term outcome in a large surgical series. Gastrointest Endosc 47:42-49, ) Pais SA, Attasaranya S, Leblanc JK, Sherman S, Schmidt CM, DeWitt J. Role of endoscopic ultrasound in the diagnosis of intraductal papillary mucinous neoplasms: correlation with surgical histopathology. Clin Gastroenterol Hepatol 5: , ) Sugiyama M, Atomi Y, Saito M. Intraductal papillary tumors of the pancreas: evaluation with endoscopic ultrasonography. Gastrointest Endosc 48: , ) Le Borgne J, de Calan L, Partensky C. Cystadenomas and cystadenocarcinomas of the pancreas: a multiinstitutional retrospective study of 398 cases. French Surgical Association. Ann Surg 230: , ) Sperti C, Pasquali C, Pedrazzoli S, Guolo P, Liessi G. Expression of mucin-like carcinoma-associated antigen in the cyst fluid differentiates mucinous from nonmucinous pancreatic cysts. Am J Gastroenterol 92: , ) Hammel P, Voitot H, Vilgrain V, Levy P, Ruszniewski P, Bernades P. Diagnostic value of CA 72-4 and carcinoembryonic antigen determination in the fluid of pancreatic cystic lesions. Eur J Gastroenterol Hepatol 10: , ) Shima Y, Mori M, Takakura N, Kimura T, Yagi T, Tanaka N. Diagnosis and management of cystic pancreatic tumours with mucin production. Br J Surg 87: ,
<30312E20C6AFC1FD303420B1E8B8EDC8AF2E687770>
 대한내과학회지 : 제 78 권제 3 호 2010 특집 (Special Review) - 췌장의낭종성질환 췌장의낭종성질환 - 수술혹은경과관찰 울산대학교의과대학내과학교실 방성조 김명환 Pancreatic cystic lesion-surgery or follow-up evaluation Sung-Jo Bang, M.D. and Myung-Hwan Kim, M.D.
대한내과학회지 : 제 78 권제 3 호 2010 특집 (Special Review) - 췌장의낭종성질환 췌장의낭종성질환 - 수술혹은경과관찰 울산대학교의과대학내과학교실 방성조 김명환 Pancreatic cystic lesion-surgery or follow-up evaluation Sung-Jo Bang, M.D. and Myung-Hwan Kim, M.D.
<30312E20C6AFC1FD303120B1E8BFEBC5C22E687770>
 대한내과학회지 : 제 78 권제 3 호 2010 특집 (Special Review) - 췌장의낭종성질환 췌장낭종성질환의개요 서울대학교의과대학내과학교실 김용태 Overview of cystic lesion of the pancreas Yong-Tae Kim, M.D., Ph.D. Department of Internal Medicine, Seoul National
대한내과학회지 : 제 78 권제 3 호 2010 특집 (Special Review) - 췌장의낭종성질환 췌장낭종성질환의개요 서울대학교의과대학내과학교실 김용태 Overview of cystic lesion of the pancreas Yong-Tae Kim, M.D., Ph.D. Department of Internal Medicine, Seoul National
untitled
 대한소화기내시경학회지 2007;35(Suppl. 1):303-307 EUS, ERCP 순천향대학교의과대학내과학교실 조영덕 췌장의낭성병변은비교적드물기는하지만최근고해상도의 CT 및 MRI 등과같은영상학적진단방법들의획기적인발전에힘입어진단율이증가하고있는추세이다. 전체췌장낭성병변중 80 90% 정도는가성낭종이차지하고있으며, 10% 정도는선천성또는단순낭종이, 그리고나머지
대한소화기내시경학회지 2007;35(Suppl. 1):303-307 EUS, ERCP 순천향대학교의과대학내과학교실 조영덕 췌장의낭성병변은비교적드물기는하지만최근고해상도의 CT 및 MRI 등과같은영상학적진단방법들의획기적인발전에힘입어진단율이증가하고있는추세이다. 전체췌장낭성병변중 80 90% 정도는가성낭종이차지하고있으며, 10% 정도는선천성또는단순낭종이, 그리고나머지
(49-54)Kjhps004.hwp
 Biliary Cystadenoma and Cystadenocarcinoma of the Liver Jae Hoon Lee, M.D., Dong Ho Choi, M.D. 1, Kyeong Geun Lee, M.D., Hwon Kyum Park M.D. and Kwang Soo Lee, M.D. Department of Surgery, College of Medicine,
Biliary Cystadenoma and Cystadenocarcinoma of the Liver Jae Hoon Lee, M.D., Dong Ho Choi, M.D. 1, Kyeong Geun Lee, M.D., Hwon Kyum Park M.D. and Kwang Soo Lee, M.D. Department of Surgery, College of Medicine,
untitled
 대한소화기내시경학회지 2007;35(Suppl. 1):308-313 췌장낭성병변 (Cystic Lesion) 의감별진단 : EUS-FNA 대구가톨릭대학교의과대학소화기내과학교실 김은영 서론최근건강에대한관심이높아지면서정기복부초음파 (abdominal ultrasound, US) 검진등의검사빈도가늘어나고전산화단층촬영술 (computed tomography, CT),
대한소화기내시경학회지 2007;35(Suppl. 1):308-313 췌장낭성병변 (Cystic Lesion) 의감별진단 : EUS-FNA 대구가톨릭대학교의과대학소화기내과학교실 김은영 서론최근건강에대한관심이높아지면서정기복부초음파 (abdominal ultrasound, US) 검진등의검사빈도가늘어나고전산화단층촬영술 (computed tomography, CT),
<313020C1F5B7CA B1E8BCD2BFAC2DB9AEBCBAC8C62E687770>
 대한내과학회지 : 제 87 권제 1 호 2014 http://dx.doi.org/10.3904/kjm.2014.87.1.61 가성낭종으로오인된급성췌장염을동반한점액성낭성종양 1 예 한림대학교의과대학한림대학교성심병원 1 소화기내과, 2 병리학과 김소연 1 문성훈 1 김동훈 2 박동선 1 안정선 1 김성열 1 김종혁 1 Mucinous Cystic Neoplasm
대한내과학회지 : 제 87 권제 1 호 2014 http://dx.doi.org/10.3904/kjm.2014.87.1.61 가성낭종으로오인된급성췌장염을동반한점액성낭성종양 1 예 한림대학교의과대학한림대학교성심병원 1 소화기내과, 2 병리학과 김소연 1 문성훈 1 김동훈 2 박동선 1 안정선 1 김성열 1 김종혁 1 Mucinous Cystic Neoplasm
<303120C1BEBCB320C0CCC5C2C0B12E687770>
 Review Article pissn 1976-3573 eissn 2288-0941 THE KOREAN JOURNAL OF PANCREAS AND BILIARY TRACT 췌장낭성병변의평가에서영상검사의역할 박범진 고려대학교안암병원영상의학과 The Role of Imaging in Evaluation: Imaging of Cystic Lesions of the
Review Article pissn 1976-3573 eissn 2288-0941 THE KOREAN JOURNAL OF PANCREAS AND BILIARY TRACT 췌장낭성병변의평가에서영상검사의역할 박범진 고려대학교안암병원영상의학과 The Role of Imaging in Evaluation: Imaging of Cystic Lesions of the
<303120C1BEBCB320C0CCC5C2C0B12E687770>
 Review Article pissn 1976-3573 eissn 2288-0941 THE KOREAN JOURNAL OF PANCREAS AND BILIARY TRACT 이태윤, 천영국, 심찬섭 건국대학교의학전문대학원내과학교실소화기병센터 Updates of Pancreatic Cystic Neoplasm: Classification and Clinical
Review Article pissn 1976-3573 eissn 2288-0941 THE KOREAN JOURNAL OF PANCREAS AND BILIARY TRACT 이태윤, 천영국, 심찬섭 건국대학교의학전문대학원내과학교실소화기병센터 Updates of Pancreatic Cystic Neoplasm: Classification and Clinical
EndoFest Korea(제4회)-편집.hwp
 C-IV. Quiz: Learning EUS from Interesting Cases Room C 췌장 성균관대학교의과대학삼성서울병원소화기내과 Jong Kyun Lee Division of Gastroenterology, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea
C-IV. Quiz: Learning EUS from Interesting Cases Room C 췌장 성균관대학교의과대학삼성서울병원소화기내과 Jong Kyun Lee Division of Gastroenterology, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea
untitled
 대한소화기학회지 2008;52:207-213 REVIEW 췌관내유두상점액종양 (IPMN) 의진단 연세대학교의료원영상의학교실방사선의과학연구소 *, 연세대학교의료원 BK21 연세의과학사업단소화기병연구소 홍혜숙 * ㆍ김명진 * Diagnosis of Pancreatic Intraductal Papillary Mucinous Neoplasm Hye-Suk Hong,
대한소화기학회지 2008;52:207-213 REVIEW 췌관내유두상점액종양 (IPMN) 의진단 연세대학교의료원영상의학교실방사선의과학연구소 *, 연세대학교의료원 BK21 연세의과학사업단소화기병연구소 홍혜숙 * ㆍ김명진 * Diagnosis of Pancreatic Intraductal Papillary Mucinous Neoplasm Hye-Suk Hong,
untitled
 대한소화기학회지 2008;51:142-146 고형가유두상종양및췌관내유두상점액종양소견을보인췌장선암종 2 예 연세대학교의과대학내과학교실및소화기병연구소, 병리학교실 * 김동현ㆍ조재희ㆍ이수현ㆍ김현기 * ㆍ방승민ㆍ송시영ㆍ정재복ㆍ박승우 Two Cases of Pancreatic Ductal Adenocarcinoma, Manifested as Solid Pseudopapillary
대한소화기학회지 2008;51:142-146 고형가유두상종양및췌관내유두상점액종양소견을보인췌장선암종 2 예 연세대학교의과대학내과학교실및소화기병연구소, 병리학교실 * 김동현ㆍ조재희ㆍ이수현ㆍ김현기 * ㆍ방승민ㆍ송시영ㆍ정재복ㆍ박승우 Two Cases of Pancreatic Ductal Adenocarcinoma, Manifested as Solid Pseudopapillary
<303220C6AFC1FD20C8ABBCBABCF72E687770>
 대한내과학회지 : 제 87 권제 3 호 2014 http://dx.doi.org/10.3904/kjm.2014.87.3.261 특집 (Special Review) - 췌장낭성종양의최신경향 췌장낭성종양의영상학적감별 순천향대학교의과대학순천향대학교서울병원영상의학과 홍성숙 Radiologic Findings of Pancreatic ystic Neoplasms Seong
대한내과학회지 : 제 87 권제 3 호 2014 http://dx.doi.org/10.3904/kjm.2014.87.3.261 특집 (Special Review) - 췌장낭성종양의최신경향 췌장낭성종양의영상학적감별 순천향대학교의과대학순천향대학교서울병원영상의학과 홍성숙 Radiologic Findings of Pancreatic ystic Neoplasms Seong
8 월대한소화기내시경학회교육자료 - 위이소성췌장에서발생한췌장염과가성낭종 이소성췌장은선천성기형의하나로, 주로위와십이지장에위치하며대부분증상없이우연히발견된다. 1,2 이소성췌장은정상췌장에서나타나는췌장염, 가성낭종, 농양, 출혈, 괴사등의병적인변화를겪을수있으며, 병변의위치와크
 8 월대한소화기내시경학회교육자료 - 위이소성췌장에서발생한췌장염과가성낭종 이소성췌장은선천성기형의하나로, 주로위와십이지장에위치하며대부분증상없이우연히발견된다. 1,2 이소성췌장은정상췌장에서나타나는췌장염, 가성낭종, 농양, 출혈, 괴사등의병적인변화를겪을수있으며, 병변의위치와크기에따라위장관폐쇄, 협착, 장중첩증등을동반하기도한다. 3-5 증상이없는경우이소성췌장에대한특별한치료가필요하지않지만증상이나합병증을동반하는경우치료가필요하며,
8 월대한소화기내시경학회교육자료 - 위이소성췌장에서발생한췌장염과가성낭종 이소성췌장은선천성기형의하나로, 주로위와십이지장에위치하며대부분증상없이우연히발견된다. 1,2 이소성췌장은정상췌장에서나타나는췌장염, 가성낭종, 농양, 출혈, 괴사등의병적인변화를겪을수있으며, 병변의위치와크기에따라위장관폐쇄, 협착, 장중첩증등을동반하기도한다. 3-5 증상이없는경우이소성췌장에대한특별한치료가필요하지않지만증상이나합병증을동반하는경우치료가필요하며,
황지웅
 Comparison of Laparoscopy and Exploration in the Distal Pancreatectomy BACKGROUND: To determine the benefits of laparoscopic surgery compared with exploration, the clinical outcomes of open and laparoscopic
Comparison of Laparoscopy and Exploration in the Distal Pancreatectomy BACKGROUND: To determine the benefits of laparoscopic surgery compared with exploration, the clinical outcomes of open and laparoscopic
untitled
 제 14 차간담췌외과연수강좌 IPMN: Natural Course and Relationship with Pancreatic Cancer 서울대학교의과대학외과학교실 장진영 서 론 1982년에처음보고된이래로췌관내유두상점액종 (intraductal papillary mucinous neoplasm: IPMN) 은현재췌장외과영역의주요질환이되었다. IPMN는주췌관또는인접한부췌관에서발생한유두상성장을하는원주세포형종양과거기서분비되는다량의점액에의한췌관의확장을특징으로하는데,
제 14 차간담췌외과연수강좌 IPMN: Natural Course and Relationship with Pancreatic Cancer 서울대학교의과대학외과학교실 장진영 서 론 1982년에처음보고된이래로췌관내유두상점액종 (intraductal papillary mucinous neoplasm: IPMN) 은현재췌장외과영역의주요질환이되었다. IPMN는주췌관또는인접한부췌관에서발생한유두상성장을하는원주세포형종양과거기서분비되는다량의점액에의한췌관의확장을특징으로하는데,
untitled
 제 14 차간담췌외과연수강좌 Practical and Easy Tips for Surgeons in the Interpretation of Radiologic Imaging: CT 울산대학교의과대학서울아산병원영상의학교실 변재호 CT는영상의학기기들중가장대표적인것으로최근눈부신발전으로그중요성이더욱강조되고있다. 대표적으로 multi-detector CT ( 이하 MDCT로함
제 14 차간담췌외과연수강좌 Practical and Easy Tips for Surgeons in the Interpretation of Radiologic Imaging: CT 울산대학교의과대학서울아산병원영상의학교실 변재호 CT는영상의학기기들중가장대표적인것으로최근눈부신발전으로그중요성이더욱강조되고있다. 대표적으로 multi-detector CT ( 이하 MDCT로함
388 The Korean Journal of Hepatology : Vol. 6. No COMMENT 1. (dysplastic nodule) (adenomatous hyperplasia, AH), (macroregenerative nodule, MR
 6 3 2000 ; 387-392 (3) Dysplastic Nodule Young Nyun Park, M.D., Chanil Park, M.D. Department of Pathology, Yonsei University College of Medicine BRIEF HISTORY 56. AST/ALT 72/73 IU/L, total bilirubin 0.7
6 3 2000 ; 387-392 (3) Dysplastic Nodule Young Nyun Park, M.D., Chanil Park, M.D. Department of Pathology, Yonsei University College of Medicine BRIEF HISTORY 56. AST/ALT 72/73 IU/L, total bilirubin 0.7
<303420C1BEBCB320B1E8C5C2C7F D E687770>
 대한내과학회지 : 제 86 권제 2 호 2014 http://dx.doi.org/10.3904/kjm.20143.86.2.152 종설 (Review) 췌관내유두상점액종양의임상적특징및예후 원광대학교의과대학내과학교실 김태현 Clinical Features and Prognosis of Intraductal Papillary Mucinous Neoplasm of
대한내과학회지 : 제 86 권제 2 호 2014 http://dx.doi.org/10.3904/kjm.20143.86.2.152 종설 (Review) 췌관내유두상점액종양의임상적특징및예후 원광대학교의과대학내과학교실 김태현 Clinical Features and Prognosis of Intraductal Papillary Mucinous Neoplasm of
untitled
 CASE REPORT THE KOREAN JOURNAL OF PANCREAS AND BILIARY TRACT 췌장가성낭종의내시경초음파유도하배액술후발생한합병증 1 예 조영걸ㆍ이태훈ㆍ박재만ㆍ박재석ㆍ전영우ㆍ박상흠ㆍ김선주ㆍ조현득 1 순천향대학교의과대학천안병원내과, 1 병리과 A Case of EUS-guided Transmural Drainge Induced Complicated
CASE REPORT THE KOREAN JOURNAL OF PANCREAS AND BILIARY TRACT 췌장가성낭종의내시경초음파유도하배액술후발생한합병증 1 예 조영걸ㆍ이태훈ㆍ박재만ㆍ박재석ㆍ전영우ㆍ박상흠ㆍ김선주ㆍ조현득 1 순천향대학교의과대학천안병원내과, 1 병리과 A Case of EUS-guided Transmural Drainge Induced Complicated
untitled
 제 14 차간담췌외과연수강좌 Pancreatobiliary Disease on Ultrasound 서울대학교의과대학영상의학과 이재영 Introduction 외과의사가알아야할기초적이고쉬운 pancreatobiliary disease의초음파소견에대해설명하고자한다. 각질환에서초음파의역할은무엇이며진단에있어어떤점에중점을두고진단을하는지감별점중가장중요한것은무엇이며주의점은무엇인지간략하게알아보고자한다.
제 14 차간담췌외과연수강좌 Pancreatobiliary Disease on Ultrasound 서울대학교의과대학영상의학과 이재영 Introduction 외과의사가알아야할기초적이고쉬운 pancreatobiliary disease의초음파소견에대해설명하고자한다. 각질환에서초음파의역할은무엇이며진단에있어어떤점에중점을두고진단을하는지감별점중가장중요한것은무엇이며주의점은무엇인지간략하게알아보고자한다.
Kaes017.hwp
 갑상선의 Poorly Differentiated (Insular) Carcinoma Insular Carcinoma: An Aggressive Subtype of Differentiated Thyroid Neoplasms Seok-Jin Nam, M.D., Sang-Dal Lee, M.D., Hal-lin Park, M.D., Young-Ryun Oh, M.D.
갑상선의 Poorly Differentiated (Insular) Carcinoma Insular Carcinoma: An Aggressive Subtype of Differentiated Thyroid Neoplasms Seok-Jin Nam, M.D., Sang-Dal Lee, M.D., Hal-lin Park, M.D., Young-Ryun Oh, M.D.
untitled
 The Korean Journal of Gastrointestinal Endoscopy Case Report 십이지장샘암종과동반된악성췌관내유두상점액종양 1 예 박경석ㆍ조재희ㆍ박태운ㆍ고근준ㆍ우명렬ㆍ정진호 * ㆍ오화은 관동대학교의과대학내과학교실, * 외과학교실, 병리학교실 A Case of Malignant Intraductal Papillary Mucinous
The Korean Journal of Gastrointestinal Endoscopy Case Report 십이지장샘암종과동반된악성췌관내유두상점액종양 1 예 박경석ㆍ조재희ㆍ박태운ㆍ고근준ㆍ우명렬ㆍ정진호 * ㆍ오화은 관동대학교의과대학내과학교실, * 외과학교실, 병리학교실 A Case of Malignant Intraductal Papillary Mucinous
<C1BEBCB320B1E8C5C2C7F62E687770>
 CASE REPORTS pissn 1976-3573 eissn 2288-0941 THE KOREAN JOURNAL OF PANCREAS AND BILIARY TRACT 정상윤 1, 김효정 1, 김재선 1, 김백희 2, 이연호 1, 유양재 1, 정용 1, 박영태 1 1 고려대학교의과대학구로병원내과학교실, 2 병리학교실 Intraductal Papillary Neoplasm
CASE REPORTS pissn 1976-3573 eissn 2288-0941 THE KOREAN JOURNAL OF PANCREAS AND BILIARY TRACT 정상윤 1, 김효정 1, 김재선 1, 김백희 2, 이연호 1, 유양재 1, 정용 1, 박영태 1 1 고려대학교의과대학구로병원내과학교실, 2 병리학교실 Intraductal Papillary Neoplasm
Kbcs002.hwp
 Does Real-time Compound Imaging Improve Evaluation of reast Cancer Compared to Conventional Sonography? o Kyoung Seo, M.D., Yu Whan Oh, M.D., Kyu Ran Cho, M.D., Young Hen Lee, M.D., Hyung Joon Noh, M.D.,
Does Real-time Compound Imaging Improve Evaluation of reast Cancer Compared to Conventional Sonography? o Kyoung Seo, M.D., Yu Whan Oh, M.D., Kyu Ran Cho, M.D., Young Hen Lee, M.D., Hyung Joon Noh, M.D.,
untitled
 CASE REPORT THE KOREAN JOURNAL OF PANCREAS AND BILIARY TRACT 송용근ㆍ박선만ㆍ김영진ㆍ김재현ㆍ최민호ㆍ장현주ㆍ계세협ㆍ이진 한림대학교의과대학내과학교실 Retroperitoneal Paraganglioma Misdiagnosed as Pancreatic Head Cancer: A Case Report Young Keun
CASE REPORT THE KOREAN JOURNAL OF PANCREAS AND BILIARY TRACT 송용근ㆍ박선만ㆍ김영진ㆍ김재현ㆍ최민호ㆍ장현주ㆍ계세협ㆍ이진 한림대학교의과대학내과학교실 Retroperitoneal Paraganglioma Misdiagnosed as Pancreatic Head Cancer: A Case Report Young Keun
한국성인에서초기황반변성질환과 연관된위험요인연구
 한국성인에서초기황반변성질환과 연관된위험요인연구 한국성인에서초기황반변성질환과 연관된위험요인연구 - - i - - i - - ii - - iii - - iv - χ - v - - vi - - 1 - - 2 - - 3 - - 4 - 그림 1. 연구대상자선정도표 - 5 - - 6 - - 7 - - 8 - 그림 2. 연구의틀 χ - 9 - - 10 - - 11 -
한국성인에서초기황반변성질환과 연관된위험요인연구 한국성인에서초기황반변성질환과 연관된위험요인연구 - - i - - i - - ii - - iii - - iv - χ - v - - vi - - 1 - - 2 - - 3 - - 4 - 그림 1. 연구대상자선정도표 - 5 - - 6 - - 7 - - 8 - 그림 2. 연구의틀 χ - 9 - - 10 - - 11 -
연하곤란
 2015.03.04 부울경소화기내시경지회 Intramucosal gastric cancer: The rate of lymph node metastasis in signet ring cell carcinoma was as low as that in welldifferentiated adenocarcinoma 인제대부산백병원 소화기내과 지삼룡 Signet ring
2015.03.04 부울경소화기내시경지회 Intramucosal gastric cancer: The rate of lymph node metastasis in signet ring cell carcinoma was as low as that in welldifferentiated adenocarcinoma 인제대부산백병원 소화기내과 지삼룡 Signet ring
( ) Jkra076.hwp
 Vol. 11, No. 4, December, 2004 Objective: Ultrasonography (USG) of joints has a unique position for the diagnosis of joint diseases. Bone surface, cartilage, periarticular soft tissue and their pathologic
Vol. 11, No. 4, December, 2004 Objective: Ultrasonography (USG) of joints has a unique position for the diagnosis of joint diseases. Bone surface, cartilage, periarticular soft tissue and their pathologic
<C3CAB7CFC1FD322DBABBB9AE2E687770>
 Advanced Course: 소화기 Ⅱ 췌담도질환에서중재적초음파내시경 (EUS) 의역할 서울대학교의과대학내과학교실 이상협 서론내시경, 초음파, 그리고컴퓨터단층촬영이지난 20년동안임상소화기학영역에서개발되었고, 이러한영상기법들을통해병리학자들에의해서만행해졌던장기의구조적인평가가현재임상에서시행될수있게되었다. 이들의빠른개발에도불구하고이들영상기법들은소화관벽과근접한구조물들에대해서는체계적인평가를할수없었다.
Advanced Course: 소화기 Ⅱ 췌담도질환에서중재적초음파내시경 (EUS) 의역할 서울대학교의과대학내과학교실 이상협 서론내시경, 초음파, 그리고컴퓨터단층촬영이지난 20년동안임상소화기학영역에서개발되었고, 이러한영상기법들을통해병리학자들에의해서만행해졌던장기의구조적인평가가현재임상에서시행될수있게되었다. 이들의빠른개발에도불구하고이들영상기법들은소화관벽과근접한구조물들에대해서는체계적인평가를할수없었다.
untitled
 CASE REPORT THE KOREAN JOURNAL OF PANCREAS AND BILIARY TRACT 복통및다발성의낭성병변으로발현된췌장결핵 1 예 안동원ㆍ김재환ㆍ윤원재ㆍ류지곤ㆍ김용태ㆍ윤용범 서울대학교의과대학내과학교실 Isolated Pancreatic Tuberculosis Presenting with Pancreatic Cystic Lesions Dong-Won
CASE REPORT THE KOREAN JOURNAL OF PANCREAS AND BILIARY TRACT 복통및다발성의낭성병변으로발현된췌장결핵 1 예 안동원ㆍ김재환ㆍ윤원재ㆍ류지곤ㆍ김용태ㆍ윤용범 서울대학교의과대학내과학교실 Isolated Pancreatic Tuberculosis Presenting with Pancreatic Cystic Lesions Dong-Won
( )Kju269.hwp
 만성세균성전립선염모델흰쥐에서 의항염효과 Anti-inflammatory Effect of Lycopene on Chronic Bacterial Prostatitis Rat Model Cho Hwan Yang, Dong Wan Sohn, Yong-Hyun Cho From the Department of Urology, The Catholic University
만성세균성전립선염모델흰쥐에서 의항염효과 Anti-inflammatory Effect of Lycopene on Chronic Bacterial Prostatitis Rat Model Cho Hwan Yang, Dong Wan Sohn, Yong-Hyun Cho From the Department of Urology, The Catholic University
SPCP.PDF
 1-1 1-2 1 1 ( ) ( ) (,, ) (,,, ), 1 ( ), ( ) ( ) 30, 30 1, +1%, 1 2 1 15 ( ) 1,, 1 3, ( ), 1 ( 210 ) 3 2, 4 9(1 ) 5 5 1 2 3, 4 5 ( ) 6 1 1 14, 21( ) 1 15 6, 21 ( ) 1 7 ( 7 )1 ( 1 ) 8 1 6 6 1, 2 ( ) 9 1
1-1 1-2 1 1 ( ) ( ) (,, ) (,,, ), 1 ( ), ( ) ( ) 30, 30 1, +1%, 1 2 1 15 ( ) 1,, 1 3, ( ), 1 ( 210 ) 3 2, 4 9(1 ) 5 5 1 2 3, 4 5 ( ) 6 1 1 14, 21( ) 1 15 6, 21 ( ) 1 7 ( 7 )1 ( 1 ) 8 1 6 6 1, 2 ( ) 9 1
<C1A63436C8B820BCBCB9CCB3AA2DC6EDC1FD2E687770>
 E-I. 개원가에서흔히보는담도췌장질환의해결 Room E 고려대학교의과대학구로병원소화기내과학교실 Bile Duct Dilatation (IHD and EHD) Jae Seon Kim Department of Internal Medicine, Guro Hospital, Korea University College of Medicine, Seoul, Korea 서론
E-I. 개원가에서흔히보는담도췌장질환의해결 Room E 고려대학교의과대학구로병원소화기내과학교실 Bile Duct Dilatation (IHD and EHD) Jae Seon Kim Department of Internal Medicine, Guro Hospital, Korea University College of Medicine, Seoul, Korea 서론
대한혜담도연구회지 1998; 3: 춰 l 장의장액성낭선종 연세대학교의과대학내과학교실및소화기병연구소병리학교실 = Abstract = 조정호 정정일 박승우 정재복박영년송시영 강진경 Serous Cystadenoma of the Pancreas Jung Ho
 대한혜담도연구회지 1998; 3: 144-149 춰 l 장의장액성낭선종 연세대학교의과대학내과학교실및소화기병연구소병리학교실 = Abstract = 조정호 정정일 박승우 정재복박영년송시영 강진경 Serous Cystadenoma of the Pancreas Jung Ho Cho, M.D., Jung 11 Chung, M.D., Seung Woo Park, M.D
대한혜담도연구회지 1998; 3: 144-149 춰 l 장의장액성낭선종 연세대학교의과대학내과학교실및소화기병연구소병리학교실 = Abstract = 조정호 정정일 박승우 정재복박영년송시영 강진경 Serous Cystadenoma of the Pancreas Jung Ho Cho, M.D., Jung 11 Chung, M.D., Seung Woo Park, M.D
 제98회 공동 건강교실 - 2005 한국인의 암 - 부인암의 예방과 치료 2005. 4.20 배 덕 수 성균관대 의대 교수 / 삼성서울병원 산부인과 김 병 기 성균관대 의대 교수 / 삼성서울병원 산부인과 목 차 자궁경부암의 예방과 치료 (강연 : 배덕수( 裵 悳 秀 ) 삼성서울병원 산부인과 교수) Ⅰ. 자궁경부암의 소개 Ⅱ. 자궁경부암의 원인 Ⅲ. 자궁경부암의
제98회 공동 건강교실 - 2005 한국인의 암 - 부인암의 예방과 치료 2005. 4.20 배 덕 수 성균관대 의대 교수 / 삼성서울병원 산부인과 김 병 기 성균관대 의대 교수 / 삼성서울병원 산부인과 목 차 자궁경부암의 예방과 치료 (강연 : 배덕수( 裵 悳 秀 ) 삼성서울병원 산부인과 교수) Ⅰ. 자궁경부암의 소개 Ⅱ. 자궁경부암의 원인 Ⅲ. 자궁경부암의
Jkbcs030(10)( ).hwp
 Treatment of Breast Fibroadenoma with Interstitial Laser Photocoagulation Doo Min Sohn, Hyo Won Lee, Tae Yun Kim, Dan Song, Sung Yong Kim, Chul Wan Lim and Min Hyuk Lee Department of Surgery, College of
Treatment of Breast Fibroadenoma with Interstitial Laser Photocoagulation Doo Min Sohn, Hyo Won Lee, Tae Yun Kim, Dan Song, Sung Yong Kim, Chul Wan Lim and Min Hyuk Lee Department of Surgery, College of
노영남
 Purpose: Delayed massive hemorrhages from pseudoaneurysm rupture of the peripancreatic large arteries, after pancreaticoduodenectomy, are fatal. We reviewed the clinical course and outcome of bleeding
Purpose: Delayed massive hemorrhages from pseudoaneurysm rupture of the peripancreatic large arteries, after pancreaticoduodenectomy, are fatal. We reviewed the clinical course and outcome of bleeding
권유진
 Malignant Peripheral Nerve Sheath Tumor of the Pancreas: A Case Report Malignant peripheral nerve sheath tumor (MPNST) is rare, soft tissue, spindle cell sarcoma of an ectomesenchymal origin. MPNSTs frequently
Malignant Peripheral Nerve Sheath Tumor of the Pancreas: A Case Report Malignant peripheral nerve sheath tumor (MPNST) is rare, soft tissue, spindle cell sarcoma of an ectomesenchymal origin. MPNSTs frequently
대한영상의학회지 2010;62:67-71 대망에서발생한췌장외의고형가성유두종양 : 증례보고 1 이염식 이영환 강유진 전세정 박성훈 윤기중 2 고형가성유두종양 (Solid pseudopapillary tumor) 은주로췌장에서발생하는저등급의악성종양으로다른장기로전이는잘하지않
 대망에서발생한췌장외의고형가성유두종양 : 증례보고 1 이염식 이영환 강유진 전세정 박성훈 윤기중 2 고형가성유두종양 (Solid pseudopapillary tumor) 은주로췌장에서발생하는저등급의악성종양으로다른장기로전이는잘하지않아비교적예후가좋다고알려져있으며췌장이외의장기에서발생하는경우는극히드물다. 저자들은고형및출혈성낭종형태로대망에서발생하여복막에결절성파종을일으킨비전형적췌장외의고형가성유두종양의영상의학적소견을문헌고찰과함께보고하고자한다.
대망에서발생한췌장외의고형가성유두종양 : 증례보고 1 이염식 이영환 강유진 전세정 박성훈 윤기중 2 고형가성유두종양 (Solid pseudopapillary tumor) 은주로췌장에서발생하는저등급의악성종양으로다른장기로전이는잘하지않아비교적예후가좋다고알려져있으며췌장이외의장기에서발생하는경우는극히드물다. 저자들은고형및출혈성낭종형태로대망에서발생하여복막에결절성파종을일으킨비전형적췌장외의고형가성유두종양의영상의학적소견을문헌고찰과함께보고하고자한다.
( ) Kjge88.hwp
 대한소화기내시경학회지 2007;35:385-390 급성담석성췌장염의중증도에영향을주는위험인자분석 원광대학교의과대학내과학교실, * 가정의학교실 오효정ㆍ김태현ㆍ최창수ㆍ권지혜ㆍ임평숙ㆍ신새론 * ㆍ최석채ㆍ나용호 Analysis of Risk Factors Associated with the Severity of Biliary Pancreatitis Hyo Jeong
대한소화기내시경학회지 2007;35:385-390 급성담석성췌장염의중증도에영향을주는위험인자분석 원광대학교의과대학내과학교실, * 가정의학교실 오효정ㆍ김태현ㆍ최창수ㆍ권지혜ㆍ임평숙ㆍ신새론 * ㆍ최석채ㆍ나용호 Analysis of Risk Factors Associated with the Severity of Biliary Pancreatitis Hyo Jeong
Jkss hwp
 급성복증을보이는감염성요막관기형 Infected Urachal Remnants with Symtoms of the Acute Abdomen: The Differential Diagnosis & Proper Management Jan Dy Lee, M.D., Chee Young Lim, M.D. 1, Hyoung Il Kim, M.D. 1, Chul Woon Chung,
급성복증을보이는감염성요막관기형 Infected Urachal Remnants with Symtoms of the Acute Abdomen: The Differential Diagnosis & Proper Management Jan Dy Lee, M.D., Chee Young Lim, M.D. 1, Hyoung Il Kim, M.D. 1, Chul Woon Chung,
untitled
 대한내과학회지 : 제 70 권부록 2 호 2006 악성변화가동반된총담관류 1 예 울산대학교의과대학서울아산병원내과학교실, 병리학교실 2 이창훈 서동완 문규 이상수 이성구 김명환 노재윤 2 =Abstract= A case of choledochocele with malignant change Chang Hun Lee, M.D., Dong Wan Seo, M.D.,
대한내과학회지 : 제 70 권부록 2 호 2006 악성변화가동반된총담관류 1 예 울산대학교의과대학서울아산병원내과학교실, 병리학교실 2 이창훈 서동완 문규 이상수 이성구 김명환 노재윤 2 =Abstract= A case of choledochocele with malignant change Chang Hun Lee, M.D., Dong Wan Seo, M.D.,
( )Jkstro011.hwp
 비인강암의방사선치료결과및생존율에관한예후인자분석 2005 2 1 2005 3 28. :, Tel: 053)250-7665, Fax: 053)250-7984 E-mail: [email protected] 정영연외 2 인 : 비인강암의예후인자분석 정영연외 2 인 : 비인강암의예후인자분석 Carcinoma of the nasopharynx treated by radiotherapy
비인강암의방사선치료결과및생존율에관한예후인자분석 2005 2 1 2005 3 28. :, Tel: 053)250-7665, Fax: 053)250-7984 E-mail: [email protected] 정영연외 2 인 : 비인강암의예후인자분석 정영연외 2 인 : 비인강암의예후인자분석 Carcinoma of the nasopharynx treated by radiotherapy
<30352EB0A3BAB4B8AE2E687770>
 The Korean Journal of Hepatology 2007 ; 13 : 571-575 DOI: 10.3350/kjhep.2007.13.4.571 이번 호의 간 병리(32) 혼합 간세포-담관세포암종 순천향대학교병원 병리과 진윤미 진소영 Combined Hepatocellular-cholangiocarcinoma Yoon-Mi Jeen, M.D. and
The Korean Journal of Hepatology 2007 ; 13 : 571-575 DOI: 10.3350/kjhep.2007.13.4.571 이번 호의 간 병리(32) 혼합 간세포-담관세포암종 순천향대학교병원 병리과 진윤미 진소영 Combined Hepatocellular-cholangiocarcinoma Yoon-Mi Jeen, M.D. and
(
 317 318 319 320 1 3 5 5 5 5 2 321 : 1.,,,,, 06 2. X-ray beam penetration (density) (contrast) 03 3. patch coating, precipitation, flaking 03 4. centering 03 5. Esophagus, cardia, fundus, body, angle, antrum,
317 318 319 320 1 3 5 5 5 5 2 321 : 1.,,,,, 06 2. X-ray beam penetration (density) (contrast) 03 3. patch coating, precipitation, flaking 03 4. centering 03 5. Esophagus, cardia, fundus, body, angle, antrum,
< C3E1B0E8C7D0BCFAB4EBC8B82DB0ADC0C7B7CF2E687770>
 Essentials of Primary Care: 소화기 무증상담낭이상소견의진단및치료 동국대학교의과대학, 동국대학교일산병원내과학교실 이준규 서론최근우리나라에서는건강검진의적극적인시행과검사방법의발달로무증상담낭이상소견이예전에비하여많이발견되고있다. 대부분은양성병변이지만일부담낭용종의경우에는진단당시에이미악성화되어있거나혹은차후에라도담낭암으로진행할수있다. 따라서자연경과및위험인자등에대한정확한이해를바탕으로하여적절한치료방침을결정하여야한다.
Essentials of Primary Care: 소화기 무증상담낭이상소견의진단및치료 동국대학교의과대학, 동국대학교일산병원내과학교실 이준규 서론최근우리나라에서는건강검진의적극적인시행과검사방법의발달로무증상담낭이상소견이예전에비하여많이발견되고있다. 대부분은양성병변이지만일부담낭용종의경우에는진단당시에이미악성화되어있거나혹은차후에라도담낭암으로진행할수있다. 따라서자연경과및위험인자등에대한정확한이해를바탕으로하여적절한치료방침을결정하여야한다.
untitled
 The Korean Journal of Gastrointestinal Endoscopy Case Report 췌담관확장을동반한바터팽대부선근종 1 예 이병욱ㆍ방제소ㆍ양수현ㆍ김지호ㆍ변종훈ㆍ시원근ㆍ이문형ㆍ최보경 서울보훈병원소화기내과 A Case of Ampullary Adenomyoma Associated with Dilatations of Pancreatic and
The Korean Journal of Gastrointestinal Endoscopy Case Report 췌담관확장을동반한바터팽대부선근종 1 예 이병욱ㆍ방제소ㆍ양수현ㆍ김지호ㆍ변종훈ㆍ시원근ㆍ이문형ㆍ최보경 서울보훈병원소화기내과 A Case of Ampullary Adenomyoma Associated with Dilatations of Pancreatic and
김범수
 Gastrointestinal stromal tumors (GISTs) are rare tumers of the alimentary tract, and these tumors arise from primitive mesenchymal cells. Duodenal GISTs comprise 4-5% of all GISTs. In this article, we
Gastrointestinal stromal tumors (GISTs) are rare tumers of the alimentary tract, and these tumors arise from primitive mesenchymal cells. Duodenal GISTs comprise 4-5% of all GISTs. In this article, we
untitled
 자가면역췌장염의임상양상 서울대학교의과대학내과학교실 류지곤 서론자가면역췌장염 (autoimmune pancreatitis, AIP) 은일반적인췌장염과달리복통은경미하며주로폐쇄성황달이주증상이며, 당뇨병이흔히동반되고췌장외장기를잘침범하는특징적인임상양상을보이는질환으로과거에는췌장암으로오인하여수술을하는경우가흔했다. 또한특징적인조직학적, 영상학적소견을보이며스테로이드치료에매우잘반응한다.
자가면역췌장염의임상양상 서울대학교의과대학내과학교실 류지곤 서론자가면역췌장염 (autoimmune pancreatitis, AIP) 은일반적인췌장염과달리복통은경미하며주로폐쇄성황달이주증상이며, 당뇨병이흔히동반되고췌장외장기를잘침범하는특징적인임상양상을보이는질환으로과거에는췌장암으로오인하여수술을하는경우가흔했다. 또한특징적인조직학적, 영상학적소견을보이며스테로이드치료에매우잘반응한다.
untitled
 SYMPOSIUM I THE KOREAN JOURNAL OF PANCREAS AND BILIARY TRACT 담관내유두상 ( 점액성 ) 종양 : 임상및내시경소견 이상수ㆍ장지웅 울산대학교의과대학서울아산병원소화기내과학교실 Intraductal Papillary (Mucinous) Neoplasm of the Bile Ducts: Clinical and Endoscopic
SYMPOSIUM I THE KOREAN JOURNAL OF PANCREAS AND BILIARY TRACT 담관내유두상 ( 점액성 ) 종양 : 임상및내시경소견 이상수ㆍ장지웅 울산대학교의과대학서울아산병원소화기내과학교실 Intraductal Papillary (Mucinous) Neoplasm of the Bile Ducts: Clinical and Endoscopic
전립선암발생률추정과관련요인분석 : The Korean Cancer Prevention Study-II (KCPS-II)
 전립선암발생률추정과관련요인분석 : The Korean Cancer Prevention Study-II (KCPS-II) 전립선암발생률추정과관련요인분석 : The Korean Cancer Prevention Study-II (KCPS-II) - i - - ii - - iii - - iv - - v - - vi - - vii - - viii - - ix - -
전립선암발생률추정과관련요인분석 : The Korean Cancer Prevention Study-II (KCPS-II) 전립선암발생률추정과관련요인분석 : The Korean Cancer Prevention Study-II (KCPS-II) - i - - ii - - iii - - iv - - v - - vi - - vii - - viii - - ix - -
08. 최호순(09-161).hwp
 대한내과학회지 : 제 77 권부록 5 호 2009 증례 09-161 내시경췌관배액술로완치된췌장 - 흉막루 한양대학교의과대학내과학교실 정명호 심성곤 조승철 이항락 이오영 윤병철 최호순 pancreaticopleural fistula cured with endoscopic pancreatic duct drainage Myung Ho Jeong, M.D., Sung
대한내과학회지 : 제 77 권부록 5 호 2009 증례 09-161 내시경췌관배액술로완치된췌장 - 흉막루 한양대학교의과대학내과학교실 정명호 심성곤 조승철 이항락 이오영 윤병철 최호순 pancreaticopleural fistula cured with endoscopic pancreatic duct drainage Myung Ho Jeong, M.D., Sung
Lumbar spine
 Lumbar spine CT 32 111 DOI : 10.3831/KPI.2010.13.2.111 Lumbar Spine CT 32 Received : 10. 05. 23 Revised : 10. 06. 04 Accepted : 10. 06. 11 Key Words: Disc herniation, CT scan, Clinical analysis The Clinical
Lumbar spine CT 32 111 DOI : 10.3831/KPI.2010.13.2.111 Lumbar Spine CT 32 Received : 10. 05. 23 Revised : 10. 06. 04 Accepted : 10. 06. 11 Key Words: Disc herniation, CT scan, Clinical analysis The Clinical
<30372EC0C7C7D0B0ADC1C22E687770>
 대한내과학회지 : 제 75 권제 3 호 2008 의학강좌 - 개원의를위한모범처방 (Current Clinical Practice) 급성췌장염의내과적치료 원광대학교내과학교실소화기내과 김태현 Medical treatment of acute pancreatitis Tae Hyeon Kim, M.D. Gastroenterology Division, Department
대한내과학회지 : 제 75 권제 3 호 2008 의학강좌 - 개원의를위한모범처방 (Current Clinical Practice) 급성췌장염의내과적치료 원광대학교내과학교실소화기내과 김태현 Medical treatment of acute pancreatitis Tae Hyeon Kim, M.D. Gastroenterology Division, Department
Hyo Sun Kim, et al. 증례 /100 mmhg, 82 /, 20 /, 36.0 C, (Murphy s sign). 4,890/mm 3, 12.8 g/dl, 378,000/mm 3, 7.08 mg/dl, 5.54 mg/dl, AST 5
 Case Report The Korean Journal of Pancreas and Biliary Tract 2016;21:96-100 http://dx.doi.org/10.15279/kpba.2016.21.2.96 pissn 1976-3573 eissn 2288-0941 중심부석회화를동반한간내담관암 1 예 1 한림대학교의과대학춘천성심병원내과, 2 울산대학교의과대학서울아산병원내과
Case Report The Korean Journal of Pancreas and Biliary Tract 2016;21:96-100 http://dx.doi.org/10.15279/kpba.2016.21.2.96 pissn 1976-3573 eissn 2288-0941 중심부석회화를동반한간내담관암 1 예 1 한림대학교의과대학춘천성심병원내과, 2 울산대학교의과대학서울아산병원내과
Very low-risk Low-risk Intermediate-risk High-risk Appendiceal mucinous tumours Mucinous adenoma Mucinou
 I. Workshop 결과에대한설문조사결과 A. 종양의행태 (behavior) 코드부여에이견이있는소화기계암에대한설문조사결과 Organ or Subject Stomach Colon Diagnosis 응답자수 ( 총 240 명 ) Low grade adenoma/dysplasia 230 10 0 1 2 3 6 무응답 High grade adenoma/dysplasia
I. Workshop 결과에대한설문조사결과 A. 종양의행태 (behavior) 코드부여에이견이있는소화기계암에대한설문조사결과 Organ or Subject Stomach Colon Diagnosis 응답자수 ( 총 240 명 ) Low grade adenoma/dysplasia 230 10 0 1 2 3 6 무응답 High grade adenoma/dysplasia
<313520C1F5B7CA B0ADC1BEBDC42DB1E8B8EDC8AF D E687770>
 대한내과학회지 : 제 84 권제 2 호 2013 http://dx.doi.org/10.3904/kjm.2013.84.2.254 신세포암의바터팽대부전이에의한급성재발성췌장염 울산대학교의과대학서울아산병원 1 내과, 2 병리과, 3 영상의학과 강종식 1 김명환 1 이성구 1 이재광 1 이민정 1 정민정 2 김진희 3 Case of cute Recurrent Pancreatitis
대한내과학회지 : 제 84 권제 2 호 2013 http://dx.doi.org/10.3904/kjm.2013.84.2.254 신세포암의바터팽대부전이에의한급성재발성췌장염 울산대학교의과대학서울아산병원 1 내과, 2 병리과, 3 영상의학과 강종식 1 김명환 1 이성구 1 이재광 1 이민정 1 정민정 2 김진희 3 Case of cute Recurrent Pancreatitis
<30352EB0A3BAB4B8AE2E687770>
 The Korean Journal of Hepatology 2008 ; 14 : 532-536 DOI: 10.3350/kjhep.2008.14.4.532 이번 호의 간 병리(36) 점액과다분비 담관세포암종 순천향대학교병원 병리과 진윤미 진소영 bstract Mucin hypersecreting cholangiocarcinoma Yoon-Mi Jeen, M.D.,
The Korean Journal of Hepatology 2008 ; 14 : 532-536 DOI: 10.3350/kjhep.2008.14.4.532 이번 호의 간 병리(36) 점액과다분비 담관세포암종 순천향대학교병원 병리과 진윤미 진소영 bstract Mucin hypersecreting cholangiocarcinoma Yoon-Mi Jeen, M.D.,
<30322EBABBB9AE2E687770>
 대한내과학회지 : 제 80 권부록 1 호 2011 개원의연수강좌 담낭용종의진단및치료가이드라인 경희대학교의과대학소화기내과학교실 동석호 서론초음파검사가건강검진등의목적으로널리시행되면서담석이나용종등의담낭질환들이많이발견되고있다. 담석의경우관련증상이뚜렷하지않으면치료하지않는것이원칙이다. 그러나담낭에서작은혹처럼보이는용종이발견되면악성을배제할수없기때문에, 그다음어찌해야할것인지종종딜레마에빠지게된다.
대한내과학회지 : 제 80 권부록 1 호 2011 개원의연수강좌 담낭용종의진단및치료가이드라인 경희대학교의과대학소화기내과학교실 동석호 서론초음파검사가건강검진등의목적으로널리시행되면서담석이나용종등의담낭질환들이많이발견되고있다. 담석의경우관련증상이뚜렷하지않으면치료하지않는것이원칙이다. 그러나담낭에서작은혹처럼보이는용종이발견되면악성을배제할수없기때문에, 그다음어찌해야할것인지종종딜레마에빠지게된다.
untitled
 REVIEW ARTICLE 외상췌장손상의치료 연세대학교의과대학외과학교실 이승환ㆍ장지영ㆍ이재길 Management of Traumatic Pancreas Injury Seung Hwan Lee, M.D., Ji Young Jang, M.D., Jae Gil Lee, M.D., Ph.D. Department of Surgery, Yonsei University
REVIEW ARTICLE 외상췌장손상의치료 연세대학교의과대학외과학교실 이승환ㆍ장지영ㆍ이재길 Management of Traumatic Pancreas Injury Seung Hwan Lee, M.D., Ji Young Jang, M.D., Jae Gil Lee, M.D., Ph.D. Department of Surgery, Yonsei University
석사논문.PDF
 ABO Rh A study on the importance of ABO and Rh blood groups information in Public Health 2000 2 1 ABO Rh A study on the importance of ABO and Rh blood groups information in Public Health 2000 2 2 ABO Rh
ABO Rh A study on the importance of ABO and Rh blood groups information in Public Health 2000 2 1 ABO Rh A study on the importance of ABO and Rh blood groups information in Public Health 2000 2 2 ABO Rh
untitled
 2009 년도대한췌담도학회춘계학술대회 Session I: Update of Chronic Pancreatitis EUS Intervention of Complications 울산대학교의과대학서울아산병원소화기내과학교실 서동완 서론만성췌장염은지속적인또는반복되는염증으로췌장의비가역적인섬유화가진행되면서췌장실질과췌관에변화가생기는질환이다. 췌장기능의소실은췌장의외분비기능과내분비기능모두에장애를초래할수있어서내분비기능의장애로인한대표적합병증이당뇨병이발생하는것이고외분비기능의장애로소화불량,
2009 년도대한췌담도학회춘계학술대회 Session I: Update of Chronic Pancreatitis EUS Intervention of Complications 울산대학교의과대학서울아산병원소화기내과학교실 서동완 서론만성췌장염은지속적인또는반복되는염증으로췌장의비가역적인섬유화가진행되면서췌장실질과췌관에변화가생기는질환이다. 췌장기능의소실은췌장의외분비기능과내분비기능모두에장애를초래할수있어서내분비기능의장애로인한대표적합병증이당뇨병이발생하는것이고외분비기능의장애로소화불량,
untitled
 Korean J Gastroenterol Vol. 66 No. 3, 154-158 http://dx.doi.org/10.4166/kjg.2015.66.3.154 pissn 1598-9992 eissn 2233-6869 REVIEW ARTICLE 내시경초음파를이용한췌장종양의국소치료 윤원재, 서동완 1 인제대학교의과대학서울백병원내과학교실, 울산대학교의과대학서울아산병원내과학교실
Korean J Gastroenterol Vol. 66 No. 3, 154-158 http://dx.doi.org/10.4166/kjg.2015.66.3.154 pissn 1598-9992 eissn 2233-6869 REVIEW ARTICLE 내시경초음파를이용한췌장종양의국소치료 윤원재, 서동완 1 인제대학교의과대학서울백병원내과학교실, 울산대학교의과대학서울아산병원내과학교실
untitled
 SYMPOSIUM THE KOREAN JOURNAL OF PANCREAS AND BILIARY TRACT Current Problems in Endoscopic Pancreatic Cytology/ Biopsy Diagnosis 이 종 균 성균관대학교 의과대학 삼성서울병원 내과학교실 Endoscopic retrograde cholangiopancreatography
SYMPOSIUM THE KOREAN JOURNAL OF PANCREAS AND BILIARY TRACT Current Problems in Endoscopic Pancreatic Cytology/ Biopsy Diagnosis 이 종 균 성균관대학교 의과대학 삼성서울병원 내과학교실 Endoscopic retrograde cholangiopancreatography
담관유두종증 447 Fig. 1. (Case 1) A computed tomographic scan shows a 4 cm sized cystic and solid mass in the segment 5 of liver (arrow). Intrahepatic bile
 대한병리학회지 : 제 37 권제 6 호 2003 The Korean Journal of Pathology. 2003; 37: 446-50 담관유두종증 - 2 예보고 - 구미진 최준혁 1 성삼병원병리과 1 영남대학교의과대학병리학교실 Biliary Papillomatosis - A Report of Two Cases - Mi Jin Gu and Joon Hyuk
대한병리학회지 : 제 37 권제 6 호 2003 The Korean Journal of Pathology. 2003; 37: 446-50 담관유두종증 - 2 예보고 - 구미진 최준혁 1 성삼병원병리과 1 영남대학교의과대학병리학교실 Biliary Papillomatosis - A Report of Two Cases - Mi Jin Gu and Joon Hyuk
<313120C1F5B7CA B7F9B4EBB0EF2DB0ADB4EBC8AF D E687770>
 대한내과학회지 : 제 86 권제 6 호 2014 http://dx.doi.org/10.3904/kjm.2014.86.6.728 고이형성증이동반된총담관류 1 예 부산대학교의과대학양산부산대학교병원내과 류대곤 김은정 안은영 송병준 강대환 A Case of Choledochocele with High-Grade Dysplasia Dae Gon Ryu, Eun Jung
대한내과학회지 : 제 86 권제 6 호 2014 http://dx.doi.org/10.3904/kjm.2014.86.6.728 고이형성증이동반된총담관류 1 예 부산대학교의과대학양산부산대학교병원내과 류대곤 김은정 안은영 송병준 강대환 A Case of Choledochocele with High-Grade Dysplasia Dae Gon Ryu, Eun Jung
<3132C1F5B7CA B1C7C7F5C8F12DBCDBC8A3C1D D E687770>
 대한내과학회지 : 제 84 권제 4 호 2013 http://dx.doi.org/10.3904/kjm.2013.84.4.551 급성담석췌장염의합병증으로발생한십이지장벽내혈종 1 예 울산대학교의과대학서울아산병원내과학교실 권혁희 최효인 전민지 송호준 이상수 정훈용 김진호 Intramural Duodenal Hematoma Caused by cute Gallstone
대한내과학회지 : 제 84 권제 4 호 2013 http://dx.doi.org/10.3904/kjm.2013.84.4.551 급성담석췌장염의합병증으로발생한십이지장벽내혈종 1 예 울산대학교의과대학서울아산병원내과학교실 권혁희 최효인 전민지 송호준 이상수 정훈용 김진호 Intramural Duodenal Hematoma Caused by cute Gallstone
06. Clinical Practice - Roadmap to diagnosis.hwp
 대한내과학회지 : 제 92 권제 2 호 2017 https://doi.org/10.3904/kjm.2017.92.2.150 Roadmap to diagnosis 증상이있는담낭담석증환자의접근법 ; 총담관담석의위험도에따라서 한림대학교의과대학한림대학교성심병원내과 문성훈 An Approach to Patients with Symptomatic Cholelithiasis
대한내과학회지 : 제 92 권제 2 호 2017 https://doi.org/10.3904/kjm.2017.92.2.150 Roadmap to diagnosis 증상이있는담낭담석증환자의접근법 ; 총담관담석의위험도에따라서 한림대학교의과대학한림대학교성심병원내과 문성훈 An Approach to Patients with Symptomatic Cholelithiasis
13 증례 KJM hwp
 대한내과학회지 : 제 94 권제 1 호 2019 https://doi.org/10.3904/kjm.2019.94.1.124 신경내분비종양과유사하게보인간과췌장에발생한악성흑색종 울산대학교의과대학서울아산병원 1 내과, 2 병리학과 노진희 1 ㆍ황인환 1 ㆍ박정하 1 ㆍ임지혜 1 ㆍ채윤 2 ㆍ홍승모 2 ㆍ김명환 1 Malignant Melanoma of the Pancreas
대한내과학회지 : 제 94 권제 1 호 2019 https://doi.org/10.3904/kjm.2019.94.1.124 신경내분비종양과유사하게보인간과췌장에발생한악성흑색종 울산대학교의과대학서울아산병원 1 내과, 2 병리학과 노진희 1 ㆍ황인환 1 ㆍ박정하 1 ㆍ임지혜 1 ㆍ채윤 2 ㆍ홍승모 2 ㆍ김명환 1 Malignant Melanoma of the Pancreas
YI Ggodme : The Lives and Diseases of Females during the Latter Half of the Joseon Dynasty as Reconstructed with Cases in Yeoksi Manpil (Stray Notes w
 497 의사학 제24권 제2호(통권 제50호) 2015년 8월 Korean J Med Hist 24 ː497-532 Aug 2015 c대한의사학회 http://dx.doi.org/10.13081/kjmh.2015.24.497 pissn 1225-505X, eissn 2093-5609 역시만필( 歷 試 漫 筆 ) 의 사례로 재구성한 조선후기 여성의 삶과 질병
497 의사학 제24권 제2호(통권 제50호) 2015년 8월 Korean J Med Hist 24 ː497-532 Aug 2015 c대한의사학회 http://dx.doi.org/10.13081/kjmh.2015.24.497 pissn 1225-505X, eissn 2093-5609 역시만필( 歷 試 漫 筆 ) 의 사례로 재구성한 조선후기 여성의 삶과 질병
untitled
 The Korean Journal of Gastrointestinal Endoscopy Case Report 총간관관상선종과동반한조기담낭암 1 예 최준호ㆍ이태훈ㆍ박상흠ㆍ심윤숙ㆍ이창균ㆍ이석호ㆍ김선주ㆍ조현득 * 순천향대학교의과대학천안병원내과학교실, * 병리학교실 A Case of Tubular Adenoma of the Common Hepatic Duct Accompanied
The Korean Journal of Gastrointestinal Endoscopy Case Report 총간관관상선종과동반한조기담낭암 1 예 최준호ㆍ이태훈ㆍ박상흠ㆍ심윤숙ㆍ이창균ㆍ이석호ㆍ김선주ㆍ조현득 * 순천향대학교의과대학천안병원내과학교실, * 병리학교실 A Case of Tubular Adenoma of the Common Hepatic Duct Accompanied
untitled
 CASE REPORT THE KOREAN JOURNAL OF PANCREAS AND BILIARY TRACT 양성담관협착진단 3 개월후간문부담관암으로확진된 1 예 전창균ㆍ장희윤ㆍ차상우ㆍ조영덕 순천향대학교의과대학내과학교실, 소화기병센터소화기연구소 A Benign Bile Duct Stricture, Finally Diagnosed as a Klatskin Tumor
CASE REPORT THE KOREAN JOURNAL OF PANCREAS AND BILIARY TRACT 양성담관협착진단 3 개월후간문부담관암으로확진된 1 예 전창균ㆍ장희윤ㆍ차상우ㆍ조영덕 순천향대학교의과대학내과학교실, 소화기병센터소화기연구소 A Benign Bile Duct Stricture, Finally Diagnosed as a Klatskin Tumor
<C1A63438C8B820BCBCB9CCB3AA2DC6EDC1FD2E687770>
 B-III. 췌담도암과관련된선행질환다루기 Room B 황은정 동석호 경희대학교의과대학내과학교실 Congenital Pancreatobiliary Anomaly Associated with Pancreatobiliary Malignancy Eun Jung Hwang, Seok Ho Dong Division of Gastroenterology and Hepatology,
B-III. 췌담도암과관련된선행질환다루기 Room B 황은정 동석호 경희대학교의과대학내과학교실 Congenital Pancreatobiliary Anomaly Associated with Pancreatobiliary Malignancy Eun Jung Hwang, Seok Ho Dong Division of Gastroenterology and Hepatology,
내시경 conference
 부울경소화기내시경학회 6월집담회 고신대학교복음병원소화기내과전임의서광일 F/63 CASE C.C) epigastric pain for 2 wks P. I) 2014.04.16 EGD at LMC adm via OPD for further evaluation. P. Hx) CASE HTN/DM/Hepatitis/Tbc (+/+/-/-) S. Hx) N-S ROS)
부울경소화기내시경학회 6월집담회 고신대학교복음병원소화기내과전임의서광일 F/63 CASE C.C) epigastric pain for 2 wks P. I) 2014.04.16 EGD at LMC adm via OPD for further evaluation. P. Hx) CASE HTN/DM/Hepatitis/Tbc (+/+/-/-) S. Hx) N-S ROS)
±è¹Ì¼º
 495 김미성 외: 자궁내막종의 초음파 소견 외 자궁내막종에서 흔히 보일 수 있는 소견들을 알아보고 가 음성군과 가양성군을 분석함으로써 초음파 진단의 함정 및 감 별진단에 도움을 주는 소견을 알아 보았다. 대상과 방법 최근 4년 동안 자궁 부속기 종괴로 수술 전 골반 초음파 검 사를 시행하여 수술 전 초음파검사에서 자궁내막종으로 진단 되고 수술로 확진된(진양성군,
495 김미성 외: 자궁내막종의 초음파 소견 외 자궁내막종에서 흔히 보일 수 있는 소견들을 알아보고 가 음성군과 가양성군을 분석함으로써 초음파 진단의 함정 및 감 별진단에 도움을 주는 소견을 알아 보았다. 대상과 방법 최근 4년 동안 자궁 부속기 종괴로 수술 전 골반 초음파 검 사를 시행하여 수술 전 초음파검사에서 자궁내막종으로 진단 되고 수술로 확진된(진양성군,
Kjhps016( ).hwp
 Surgical Extent and Types in Pancreatic Cancer Song Cheol Kim, M.D. Department of Surgery, Ulsan University College of Medicine & Asan Medical Center, Seoul, Korea Pancreatic cancer continues to pose a
Surgical Extent and Types in Pancreatic Cancer Song Cheol Kim, M.D. Department of Surgery, Ulsan University College of Medicine & Asan Medical Center, Seoul, Korea Pancreatic cancer continues to pose a
제5회 가톨릭대학교 의과대학 마취통증의학교실 심포지엄 Program 1 ANESTHESIA (Room 2층 대강당) >> Session 4 Updates on PNB Techniques PNB Techniques for shoulder surgery: continuou
 제5회 가톨릭대학교 의과대학 마취통증의학교실 심포지엄 (Room 2층 대강당) >> Session 4 Updates on PNB Techniques PNB Techniques for shoulder surgery: continuous vs single injection, interscalene vs supraclavicular approach 의정부성모병원
제5회 가톨릭대학교 의과대학 마취통증의학교실 심포지엄 (Room 2층 대강당) >> Session 4 Updates on PNB Techniques PNB Techniques for shoulder surgery: continuous vs single injection, interscalene vs supraclavicular approach 의정부성모병원
<30325FB0EDB5BFC8F12E687770>
 REVIEW ARTICLE pissn 1976-3573 eissn 2284-0941 THE KOREAN JOURNAL OF PANCREAS AND BILIARY TRACT 고동희, 김종혁, 이진, 최호순 1 한림대학교의과대학내과학교실, 1 한양대학교의과대학내과학교실 Clinical Practice Guidelines for Acute Pancreatitis:
REVIEW ARTICLE pissn 1976-3573 eissn 2284-0941 THE KOREAN JOURNAL OF PANCREAS AND BILIARY TRACT 고동희, 김종혁, 이진, 최호순 1 한림대학교의과대학내과학교실, 1 한양대학교의과대학내과학교실 Clinical Practice Guidelines for Acute Pancreatitis:
Review Article The Korean Journal of Pancreas and Biliary Tract 2014;19: pissn eissn 22
 Review Article The Korean Journal of Pancreas and Biliary Tract 2014;19:121-127 http://dx.doi.org/10.15279/kpba.2014.19.3.121 pissn 1976-3573 eissn 2288-0941 유두부종양의진단과치료에서내시경의역할 연세대학교의과대학내과학교실소화기내과, 소화기병연구소
Review Article The Korean Journal of Pancreas and Biliary Tract 2014;19:121-127 http://dx.doi.org/10.15279/kpba.2014.19.3.121 pissn 1976-3573 eissn 2288-0941 유두부종양의진단과치료에서내시경의역할 연세대학교의과대학내과학교실소화기내과, 소화기병연구소
16(2)-7(p ).fm
 w wz 16«2y Kor. J. Clin. Pharm., Vol. 16, No. 2. 2006 ü t xy y w tœ ½ BÁ x BC B y w w w C y w w w Current Status and Expectations of Orphan Drugs in Korea -In point of supplying medicines for the rare
w wz 16«2y Kor. J. Clin. Pharm., Vol. 16, No. 2. 2006 ü t xy y w tœ ½ BÁ x BC B y w w w C y w w w Current Status and Expectations of Orphan Drugs in Korea -In point of supplying medicines for the rare
untitled
 대한소화기학회지 2009;53:383-387 DOI: 10.4166/kjg.2009.53.6.383 범발담관침범을동반한자가면역췌장염 1 예 동아대학교의과대학내과학교실, 영상의학교실 * 이창민ㆍ노명환ㆍ정창길ㆍ원종진ㆍ백양현ㆍ이성욱ㆍ최석렬ㆍ조진한 * A Case of Autoimmune Pancreatitis Combined with Extensive Involvement
대한소화기학회지 2009;53:383-387 DOI: 10.4166/kjg.2009.53.6.383 범발담관침범을동반한자가면역췌장염 1 예 동아대학교의과대학내과학교실, 영상의학교실 * 이창민ㆍ노명환ㆍ정창길ㆍ원종진ㆍ백양현ㆍ이성욱ㆍ최석렬ㆍ조진한 * A Case of Autoimmune Pancreatitis Combined with Extensive Involvement
<303320C6AFC1FD303320B3B2B1A4BFEC2DBCDBC5C2C1D82E687770>
 대한내과학회지 : 제 89 권제 5 호 2015 http://dx.doi.org/10.3904/kjm.2015.89.5.507 특집 (Special Review) - 췌담도질환의최신지견 내시경초음파유도하중재시술 울산대학교의과대학서울아산병원소화기내과 남광우 송태준 Endoscopic Ultrasound Guided Intervention Kwangwoo Nam
대한내과학회지 : 제 89 권제 5 호 2015 http://dx.doi.org/10.3904/kjm.2015.89.5.507 특집 (Special Review) - 췌담도질환의최신지견 내시경초음파유도하중재시술 울산대학교의과대학서울아산병원소화기내과 남광우 송태준 Endoscopic Ultrasound Guided Intervention Kwangwoo Nam
Jung YH, et al. 228 증 례 진전은 없었다. 검사 소견: 말초혈액검사나 혈청 생화학검사는 정상이었고, 갑상 환자: 55세, 여자 선기능검사는 갑상선자극호르몬(thyroid stimulating hormone) 1.68 주소: 갑상선 우연종 µiu/ml (
 Endocrinol Metab 27(3):227-231, September 2012 CASE REPORT 갑상선유두암의 전이와 혼동되었던 난소갑상선종 1예 정영희 정성민 이종민 장이선 이인석 김종옥 1 김혜수 가톨릭대학교 의과대학 대전성모병원 내과, 병리과 1 A Case of Incidental Struma Ovarii Confounded with the
Endocrinol Metab 27(3):227-231, September 2012 CASE REPORT 갑상선유두암의 전이와 혼동되었던 난소갑상선종 1예 정영희 정성민 이종민 장이선 이인석 김종옥 1 김혜수 가톨릭대학교 의과대학 대전성모병원 내과, 병리과 1 A Case of Incidental Struma Ovarii Confounded with the
untitled
 대한내과학회지 : 제 70 권제 6 호 2006 증상을동반한거대가성낭종을형성한이소성췌장 1 예 충북대학교의과대학내과학교실, 해부병리학교실 2 박성순 신윤미 임성우 김석형 2 전원중 박선미 윤세진 =Abstract= A case of symptomatic heterotopic pancreas with huge pseudocyst formation Sung Soon
대한내과학회지 : 제 70 권제 6 호 2006 증상을동반한거대가성낭종을형성한이소성췌장 1 예 충북대학교의과대학내과학교실, 해부병리학교실 2 박성순 신윤미 임성우 김석형 2 전원중 박선미 윤세진 =Abstract= A case of symptomatic heterotopic pancreas with huge pseudocyst formation Sung Soon
장영주.hwp
 대한내과학회지 : 제 80 권부록 2 호 2011 담도암과감별이어려웠던국소형자가면역성췌장염 한국원자력의학원 1 내과, 2 외과, 3 병리학과 장영주 1 양기영 1 김상범 2 박선후 3 안영 1 양재현 1 이종환 1 Focal-Type Autoimmune Pancreatitis Mimicking Cholangiocarcinoma Young Joo Jang 1,
대한내과학회지 : 제 80 권부록 2 호 2011 담도암과감별이어려웠던국소형자가면역성췌장염 한국원자력의학원 1 내과, 2 외과, 3 병리학과 장영주 1 양기영 1 김상범 2 박선후 3 안영 1 양재현 1 이종환 1 Focal-Type Autoimmune Pancreatitis Mimicking Cholangiocarcinoma Young Joo Jang 1,
untitled
 The Korean Journal of Gastrointestinal Endoscopy Room D Prevention for Post-ERCP Pancreatitis: Interventional Aspect 울산대학교의과대학서울아산병원소화기내과학교실 서론 ERCP후발생하는췌장염 (post-ercp pancreatitis, PEP) 은드물지않은시술후합병증이면서위중한결과를초래할수있다.
The Korean Journal of Gastrointestinal Endoscopy Room D Prevention for Post-ERCP Pancreatitis: Interventional Aspect 울산대학교의과대학서울아산병원소화기내과학교실 서론 ERCP후발생하는췌장염 (post-ercp pancreatitis, PEP) 은드물지않은시술후합병증이면서위중한결과를초래할수있다.
대한영상의학회지 2010;62: 자기공명영상에서보이는난소성숙낭기형종의조영증강고형성분 : 악성세포전환을의미하는가? 1 송명규 김경아 이창희 최재웅 이종미 김윤환 박철민 목적 : MR 영상에서보이는난소의양성성숙낭기형종의조영증강고형성분에대해알아보고자하였다. 대상
 대한영상의학회지 2010;62:271-276 자기공명영상에서보이는난소성숙낭기형종의조영증강고형성분 : 악성세포전환을의미하는가? 1 송명규 김경아 이창희 최재웅 이종미 김윤환 박철민 목적 : MR 영상에서보이는난소의양성성숙낭기형종의조영증강고형성분에대해알아보고자하였다. 대상과방법 : 수술전 MR 영상을시행하였고병리학적으로양성난소성숙낭기형종으로진단된 32명의환자중조영증강고형성분을보였던
대한영상의학회지 2010;62:271-276 자기공명영상에서보이는난소성숙낭기형종의조영증강고형성분 : 악성세포전환을의미하는가? 1 송명규 김경아 이창희 최재웅 이종미 김윤환 박철민 목적 : MR 영상에서보이는난소의양성성숙낭기형종의조영증강고형성분에대해알아보고자하였다. 대상과방법 : 수술전 MR 영상을시행하였고병리학적으로양성난소성숙낭기형종으로진단된 32명의환자중조영증강고형성분을보였던
Can032.hwp
 Chromosomal Alterations in Hepatocellular Carcinoma Cell Lines Detected by Comparative Genomic Hybridization Sang Jin Park 1, Mahn Joon Ha, Ph.D. 1, Hugh Chul Kim, M.D. 2 and Hyon Ju Kim, M.D. 1 1 Laboratory
Chromosomal Alterations in Hepatocellular Carcinoma Cell Lines Detected by Comparative Genomic Hybridization Sang Jin Park 1, Mahn Joon Ha, Ph.D. 1, Hugh Chul Kim, M.D. 2 and Hyon Ju Kim, M.D. 1 1 Laboratory
<30382EC0C7C7D0B0ADC1C22E687770>
 대한내과학회지: 제 76 권 제 2 호 2009 의학강좌-개원의를 위한 모범처방(Current Clinical Practice) 간기능검사의 이해와 적용 인제대학교 의과대학 일산백병원 내과학교실 김 경 아 Understanding and application of liver function tests Kyung-Ah Kim, M.D. Department of
대한내과학회지: 제 76 권 제 2 호 2009 의학강좌-개원의를 위한 모범처방(Current Clinical Practice) 간기능검사의 이해와 적용 인제대학교 의과대학 일산백병원 내과학교실 김 경 아 Understanding and application of liver function tests Kyung-Ah Kim, M.D. Department of
<B9ABC1A62D312E696E6464>
 Korean Journal of HBP Surgery Vol. 13, No 2, June 원저 단일기관에서경험한신세포암의췌장전이치료경험 Renal Carcinoma Cell Metastasis into Pancreas : A Single Center Experience Introduction: Renal cell carcinoma (RCC) is a relative
Korean Journal of HBP Surgery Vol. 13, No 2, June 원저 단일기관에서경험한신세포암의췌장전이치료경험 Renal Carcinoma Cell Metastasis into Pancreas : A Single Center Experience Introduction: Renal cell carcinoma (RCC) is a relative
Jkbcs016(92-97).hwp
 Expression of bcl-2 and Apoptosis and Its Relationship to Clinicopathological Prognostic Factors in Breast Cancer - A Study with Long Term Follow-up correlated with the survival rate.(journal of Korean
Expression of bcl-2 and Apoptosis and Its Relationship to Clinicopathological Prognostic Factors in Breast Cancer - A Study with Long Term Follow-up correlated with the survival rate.(journal of Korean
ºÎÁ¤¸ÆV10N³»Áö
 case of brugada syndrome presented as chest pain STRCT rugada syndrome was described in 1992 as a new clinical entity characterized by electrocardiographic STsegment elevation in the right precordial leads
case of brugada syndrome presented as chest pain STRCT rugada syndrome was described in 1992 as a new clinical entity characterized by electrocardiographic STsegment elevation in the right precordial leads
